|
 |


- Search
| Int Neurourol J > Volume 27(Suppl 1); 2023 > Article |
|
ABSTRACT
Purpose
This clinical study sought to evaluate the possible clinical effectiveness and practicality of URINO, an innovative, incisionless, and disposable intravaginal device, designed for patients suffering from stress urinary incontinence.
Methods
A prospective, multicenter, single-arm clinical trial was carried out, involving women diagnosed with stress urinary incontinence who used a self-inserted, disposable intravaginal pessary device. Comparisons were made between the results of the 20-minute pad-weight gain (PWG) test at baseline and visit 3, where the device was applied. After 1 week of device usage, compliance, satisfaction, the sensation of a foreign body, and adverse events were assessed.
Results
Out of 45 participants, 39 completed the trial and expressed satisfaction within the modified intention-to-treat group. The average 20-minute PWG of participants was 17.2±33.6 g at baseline and significantly dropped to 5.3±16.2 g at visit 3 with device application. A total of 87.2% of participants exhibited a reduction ratio of PWG by 50% or more, surpassing the clinical trial success benchmark of 76%. The mean compliance was recorded as 76.6%±26.6%, the average visual analogue scale score for patient satisfaction was 6.4±2.6, and the sensation of a foreign body, measured on a 5-point Likert scale, was 3.1±1.2 after 1 week of device use. No serious adverse events were reported; there was 1 instance of microscopic hematuria and 2 cases of pyuria, all of which recovered.
Conclusions
The investigated device demonstrated significant clinical effectiveness and safety for patients with stress urinary incontinence. It was easy to use, showing favorable patient compliance. We propose that these disposable intravaginal pessaries could potentially be an alternative treatment for patients with stress urinary incontinence who are seeking nonsurgical options or are unable to undergo surgery.
Stress urinary incontinence (SUI) is characterized by the involuntary loss of urine during physical effort, exertion, or when sneezing or coughing [1]. Reports consistently indicate that SUI can have both physical and psychological impacts, including financial issues and quality of life concerns, with a prevalence rate of 25% to 50% among the female population.
The weakening of the urinary sphincter muscles or pelvic floor muscles (PFMs) that support the urethra can lead to SUI. This is often due to factors such as vaginal delivery, aging, body weight, and pelvic surgery [2-5]. Therefore, treatment options for SUI aim to address this anatomical weakening and include conservative measures such as PFM exercises, behavioral modifications, vaginal pessary-like devices, and surgery [6,7]. Current guidelines recommend 4 different surgical options, with tension-free vaginal and obturator tapes primarily used to treat severe SUI due to their proven efficacy and safety [4,8]. However, after the U.S. Food and Drug Administration (FDA) reclassified meshes used for pelvic organ prolapse repair as class III devices, it raised similar concerns for midurethral slings. Patients with mild to moderate symptoms who prefer conservative methods, or those at high operative risk, still have limited treatment options. In this context, some pessary-like devices that support and train the PFM have been developed [7,9-11].
URINO (RimHealthcare, Seoul, Korea), a novel incision-free and disposable investigational device, serves as a preventative tool for urinary incontinence. It is designed to be used daily for up to 8 hours. The device is inserted about 3 cm into the vagina where it supports the PFM and the midurethra, reinforcing the urethral sphincter. The device works to prevent urinary incontinence when intrabdominal pressure increases, a function similar to that of a midurethral sling operation (Fig. 1). Moreover, it is designed to avoid inducing urge incontinence, as the device’s insertion part and the external hook are integrated and designed not to compress the bladder directly. An empty space inside the device minimizes foreign body sensation or pressure to the vagina. The device is composed of a main body and strap, which facilitate easy insertion and removal. This study aims to investigate the potential clinical efficacy and feasibility of URINO for patients with SUI.
We designed and conducted a prospective, multicenter, single-arm clinical study, where participants served as their own controls, to evaluate the efficacy and safety of an investigational pessary device for patients with SUI. The study, approved by the Internal Review Board (IRB) at 2 separate institutions—Chungnam National University Daejeon Hospital (IRB No.: CNUH 2022-06-052) and Chungnam National University Sejong Hospital (IRB No.: CNUSH 2022-04-012)—ensured all participants provided written informed consent before undertaking any study procedures. The study was registered as a clinical trial (KCT0008369). Technical support was provided by RimHealthcare, South Korea, the manufacturer of the investigational device.
The recruitment of subjects occurred from July 2022 to January 2023 across the 2 institutions. The criteria for eligibility included nonpregnant women aged between 30 to 79 years, diagnosed with SUI for over 3 months by expert urologists, with an objective 20-minute pad-weight gain (PWG) test result of more than 1 g, and a bladder filled with over 250 mL of urine. Participants were also required to have no contraindications for using a pessary, no advanced pelvic organ prolapse, the ability to insert and remove the device independently, and willingness to participate in the study. The exclusion criteria were any active urinary tract or vaginal infection within the last 6 months, as determined by urinalysis and a vaginal swab (wet mount and culture), respectively. We also excluded participants with a history of surgery for SUI, those with urgency or mixed urinary incontinence, and those who had undergone surgery for pelvic or adjacent organs where the device is inserted within the last 6 months (including vaginal delivery). Participants with unhealed scars, allergies, and/or musculoskeletal diseases at the site of contact with the device at the time of screening were also excluded. Those with pelvic organ prolapse (greater than grade III), those pregnant or non-menopausal participants who did not agree to adhere to the contraceptive regimen suggested for this clinical trial, and those deemed unfit for this clinical trial by a clinician were also excluded from the study.
Potential participants for the study were identified, consented, and then completed a screening visit (visit 1), which encompassed a comprehensive medical history review, a physical examination, a urine pregnancy test, laboratory tests, and urinalysis. Candidates who successfully passed the screening, including the physical examination, were enrolled and undertook a 20-minute PWG test. At visit 2, these subjects received the clinical trial devices along with instructions for their proper use. Those who could independently apply the device without any contraindications were deemed eligible and given the investigational devices to use for a 7-day treatment period, for up to 8 hours each day. After completing the 7-day device application, participants were asked to return for visit 3, where they underwent further tests, including a physical examination, a urine pregnancy test, laboratory tests, and urinalysis. In addition, participants retook the 20-minute PWG test while the device was in place. Compliance was assessed based on patient diaries, satisfaction was gauged using a visual analogue scale (VAS) questionnaire, and the sensation of a foreign body was evaluated on a 5-point Likert scale. Participants were then required to return a week later (visit 4) and complete a physical examination, laboratory tests, and urinalysis. Adverse events were documented and evaluated at all stages of the study.
In accordance with the FDA guidance for clinical investigations of devices indicated for the treatment of urinary incontinence, a clinically meaningful level of improvement in PWG is defined as a reduction greater than 50% from the baseline. Therefore, a reduction of at least 50% in PWG was considered a success [12]. To verify the device’s efficacy, the 20-minute PWG test was performed twice: during visit 1 and visit 3. Before each test, the residual urine volume was confirmed to be 250 mL or more using ultrasound [13-15]. At the baseline (visit 1), a 20-minute PWG test was conducted without the device, and any urinary incontinence of 1 g or more was deemed significant. At visit 3, the PWG test was repeated with the device in place, and the percentage reduction of PWG compared to the result at visit 1 was evaluated.
Patient satisfaction was gauged using a VAS scale ranging from 0 to 10, with 0 indicating complete dissatisfaction and 10 denoting extreme satisfaction. After 7 days of device usage, participants were asked to select a whole number between 1 and 10 that best reflected their level of satisfaction.
A 5-point Likert scale was used to assess any sensation of a foreign body, with 5 indicating no sensation of a foreign body and 1 indicating a severe sensation of a foreign body.
In a previous study by Duenas-Garcia et al. [9], 54.1% of participants demonstrated a reduction in PWG of more than 50%. Using this result, we set our reference value at 0.54 and anticipated a new value of 0.76, hypothesizing that 76% of our participants would show a 50% or greater reduction in PWG. Consequently, we used the following formula to calculate our sample size:
The sample size was adjusted to allow a 10% (4 patients) loss to follow-up.
All inferential analyses were carried out on the modified intention-to-treat (mITT) population. P-values less than 0.05 were deemed statistically significant and all statistical tests were 2-tailed unless otherwise specified. Continuous variables were summarized using descriptive statistics, which included the mean, standard deviation, minimum, maximum, and median. The Shapiro-Wilk test, Kolmogorov-Smirnov test, and Q-Q plot were utilized to illustrate the distribution of the collected data. The 1-sample z-test for the proportion of PWG reduction was conducted for the primary efficacy assessment. The paired t-test was used for data that were normally distributed, and the Wilcoxon test was applied to data that were not normally distributed. The latest version of R ver. 4.2.3 (R Development Core Team, Vienna, Austria) was used for these analyses.
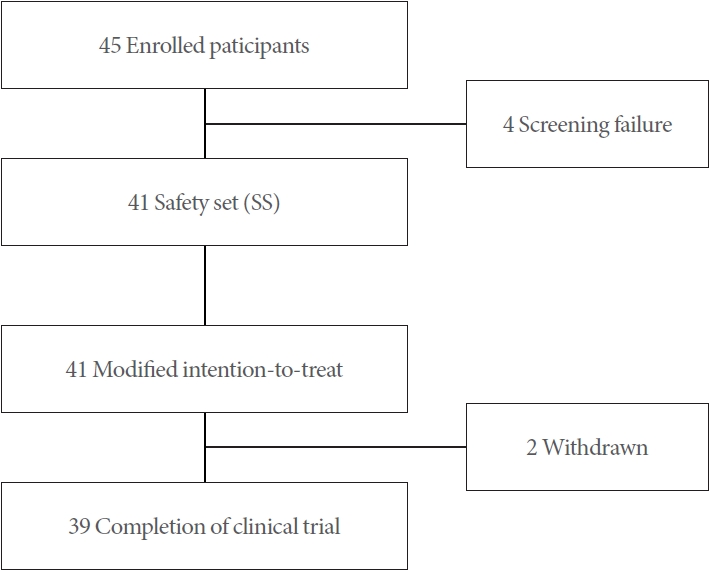
In total, 45 participants across all clinical trial sites were evaluated for study inclusion. Of these, 4 did not pass the initial screening, and 2 withdrew their consent to participate in the study (Fig. 2). The average age of the participants was 55.0±11.7 years, with a mean height of 156.9±5.6 cm, and an average weight of 59.7± 8.1 kg. The participants’ mean body mass index was 24.3±3.1 kg/m2, and their mean 20-minute PWG at baseline was 17.2± 33.6 g (Table 1).
To evaluate the device’s effectiveness, we compared the results of the 20-minute PWG at both visit 1 and visit 3 (Table 2). The average 20-minute PWG at baseline (visit 1) was 17.2±33.6 g for the participants. After using the device, the PWG significantly dropped to 5.3±16.2 g at visit 3 (P<0.001). When comparing the 20-minute PWG test results at visit 3 to the baseline, 34 out of the total 39 subjects, or 87.2% of the mITT group, demonstrated a reduction of 50% or more in PWG. This result surpassed the clinical trial success benchmark of 76% (Fig. 3).
The average compliance among the 41 patients in the mITT group was 76.6%±26.6%, with a range from 25% to 100% (Fig. 4A). However, when restricted to the per-protocol group, the average compliance was 98.3%±4.6%, with a range from 84% to 100%, demonstrating high compliance (data not shown in this article). The mean VAS score assessing patient satisfaction after 1 week of device use was 6.4±2.6, indicating positive patient satisfaction with device use (Fig. 4B). The foreign body sensation reported by the subjects after one week of device use was assessed using a 5-point Likert scale, yielding an average score of 3.1±1.2 (Fig. 4C).
A supplementary subanalysis was undertaken to determine if certain subdivisions of baseline demographics and clinical characteristics demonstrated greater device efficacy or notable differences in patient satisfaction, foreign body sensation, and device compliance (Table 3). The subanalysis found no significant differences in efficacy, satisfaction, and compliance across the subdivisions. However, for foreign body sensation, participants in their 40s reported less foreign body sensation than those in their 70s (mean difference, 2.000; 95% confidence interval confidence interval [CI], 0.18–3.82; P=0.025). Moreover, participants with a body mass index (BMI) between 18.5 and 23 kg/m2 tended to report less foreign body sensation than those with a BMI between 25 and 30 kg/m2, although this difference was not statistically significant (mean difference, 1.157; 95% CI: -0.09 to 2.40; P=0.077).
The application of the device did not impact vital signs. A brief increase in blood pressure was observed in 2 patients, but this normalized subsequently. In total, 12 participants (29.3%) reported one or more adverse events, totaling 13 events, although no serious adverse events were recorded. Five participants experienced pain associated with the device, but they found it manageable. One instance of microscopic hematuria (urine positive for red blood cells) persisted throughout the clinical trial (3–5 red blood cells per high-power field), while another resolved (Table 4). Two instances of clinically symptomatic pyuria (urine positive for white blood cells) were detected, both of which improved with conservative treatment. All other abnormalities resolved.
This clinical trial aimed to ascertain the efficacy and safety of a novel investigational disposable pessary-like device for patients with SUI. Out of 45 individuals who consented to participate, 4 were excluded during screening, resulting in a total of 41 participants for the trial. Among them, 2 withdrew their consent, leading to their drop-out. Importantly, no participants left the study due to significant adverse events related to device use.
Ever since the introduction of the tension-free vaginal tape procedure, transobturator types of midurethral slings have become the standard surgical treatment due to their minimally invasive nature and proven efficacy for patients with SUI [16-18]. However, concerns for several complications from midurethral sling use, such as complications of general anesthesia, incidence of bladder injury, postoperative voiding dysfunction and groin or thigh pain, still exist [19,20]. Therefore, a conservative approach should be initially considered in women with mild symptoms of SUI.
Historically, pessaries have been utilized for centuries to manage pelvic organ prolapse [21]. Recently, a variety of new pessary types have been introduced, designed to support the anterior vaginal wall, urethra, and bladder neck, thereby preventing urinary leakage during increases in intra-abdominal pressure [22]. The Nolix devices investigated in 2021 demonstrated an average reduction in PWG of 79.4%, with minimal serious side effects and relatively good compliance from participants [10]. Another innovative device, developed by Rinovum, achieved more than a 50% reduction in daily PWG, daily leakage episodes, or both, in 71% of participants. Participants reported improvements in quality of life and found the device easy to use [9]. Past studies have also reported similar efficacy in SUI patients using pessary-like devices [11,23,24]. Our study’s findings corroborate these results, showing that this novel device effectively reduces PWG by more than 50% in 87.2% of participants. Although vaginal irritation and pain were common complaints for up to 45% of patients with early investigational devices [9,11,24], the new pessary-type device is made of Thermo Plastic Rubber material, which is well tolerated and enables easy insertion or removal of the device with minimal foreign body sensation. Moreover, while early investigation devices had reports of urinary tract or vaginal infections [11], the URINO device, which is recommended for 8 hours of daily use, was not associated with any infection among the study participants.
The FDA advises that clinical trials evaluating the efficacy of investigational devices intended for the treatment of urinary incontinence should consider longer periods of assessment. This includes measuring PWG during up to 12 hours of daily use over a week or more and tracking leakage episodes over several weeks [12]. In this study, however, we determined the device’s efficacy through an objective 20-minute PWG test, which reliably quantified urine leakage output, in contrast to less reliable subjective reports. For patients with mild to moderate symptoms of SUI who are reluctant to undergo surgery, this device, with its proven efficacy, can be employed according to the patient’s preference.
Despite the absence of significant differences in efficacy, satisfaction, and compliance according to subdivisions of the population in this study’s subanalysis, further research is required. Future studies should focus on individualized size for optimal fit and the need to confirm long-term compliance and potential adverse events.
In conclusion, the novel disposable pessary device for patients with SUI demonstrated commendable clinical efficacy and safety, as well as ease of use with favorable patient compliance. We believe that disposable intravaginal pessaries could become a future alternative treatment for patients with SUI who are seeking nonsurgical treatments or are unable to undergo surgery.
NOTES
Research Ethics
This study was conducted with the approval of the Chungnam National University Hospital and the Chungnam National University Sejong Hospital Institutional Review Board (IRB No.: CNUH 2022-06-052 and CNUSH 2022-04-012). Patients participated voluntarily in this study and provided written informed consent. This study adhered to the ethical principles stated in the Declaration of Helsinki and International Conference on Harmonization (ICH) Guidelines. To protect the rights, interests, and safety of subjects, the study was carried out in accordance with Korean Good Clinical Practice (KGCP) standards and the International Conference on Harmonization-Good Clinical Practice (ICH-GCP).
Conflict of Interest
This study received research grant support from RimHealthcare. The funding source had no influence on the study’s design or implementation; data collection, management, analysis, or interpretation; manuscript preparation, review, or approval; or the decision to submit the manuscript for publication. The authors declare no conflict of interest.
REFERENCES
1. D’Ancona C, Haylen B, Oelke M, Abranches-Monteiro L, Arnold E, Goldman H, et al. The International Continence Society (ICS) report on the terminology for adult male lower urinary tract and pelvic floor symptoms and dysfunction. Neurourol Urodyn 2019;38:433-77. PMID: 30681183



2. Chong EC, Khan AA, Anger JT. The financial burden of stress urinary incontinence among women in the United States. Curr Urol Rep 2011;12:358-62. PMID: 21847532



3. Chow PM, Chuang YC, Hsu KCP, Shen YC, Liu SP. Impact of female stress urinary incontinence on quality of life, mental health, work limitation, and healthcare seeking in China, Taiwan, and South Korea (LUTS Asia): results from a cross-sectional, population-based study. Int J Womens Health 2022;14:1871-80. PMID: 36597480




4. Kim A, Kim S, Kim HG. Current overview of surgical options for female stress urinary incontinence. Int Neurourol J 2020;24:222-30. PMID: 33017893




5. Rogers RG. Clinical practice. Urinary stress incontinence in women. N Engl J Med 2008;358:1029-36. PMID: 18322284


6. Bø K. Urinary incontinence, pelvic floor dysfunction, exercise and sport. Sports Med 2004;34:451-64. PMID: 15233598


7. Titman SC, Radley SC, Gray TG. Self-management in women with stress incontinence: strategies, outcomes and integration into clinical care. Res Rep Urol 2019;11:111-21. PMID: 31114767


8. Kobashi KC, Albo ME, Dmochowski RR, Ginsberg DA, Goldman HB, Gomelsky A, et al. Surgical treatment of female stress urinary incontinence: AUA/SUFU guideline. J Urol 2017;198:875-83. PMID: 28625508


9. Duenas-Garcia OF, Shapiro RE, Gaccione P. Safety and efficacy of a disposable vaginal device for stress urinary incontinence. Female Pelvic Med Reconstr Surg 2021;27:360-4. PMID: 32453209



10. Naor MS, Kaploun A, Friedman B. A feasibility study with a novel, dynamic, and disposable over-the-counter device for the management of stress urinary incontinence. Neurourol Urodyn 2021;40:653-8. PMID: 33348425



11. Ziv E, Stanton SL, Abarbanel J. Efficacy and safety of a novel disposable intravaginal device for treating stress urinary incontinence. Am J Obstet Gynecol 2008;198:594.e1-7. PMID: 18377862


12. U.S. Food and Drug Administration (FDA). Guidance for industry and Food and Drug Administration staff: clinical investigations of devices indicated for the treatment of urinary incontinence. Silver Spring (MD): U.S. Food and Drug Administration (FDA); 2016.
13. Wu WY, Sheu BC, Lin HH. Comparison of 20-minute pad test versus 1-hour pad test in women with stress urinary incontinence. Urology 2006;68:764-8. PMID: 17070349


14. Prudencio CB, de Azevedo Ferreira L, Gimenez MM, de Aquino Nava GT, Bortolini MAT, Castro RA, et al. Is there a correlation between a 20-min pad-test and subjective urine leakage amount? Int Urogynecol J 2021;32:2857-62. PMID: 34459926



15. Fajar Marta K, Moegni F. Level of agreement and acceptance of the 20-Minute versus 60-Minute sanitary pad test as a method for measuring the severity of stress urinary incontinence: randomised crossover trial. J Obstet Gynaecol 2022;42:1251-4. PMID: 34558386


16. Ulmsten U, Falconer C, Johnson P, Jomaa M, Lannér L, Nilsson CG, et al. A multicenter study of tension-free vaginal tape (TVT) for surgical treatment of stress urinary incontinence. Int Urogynecol J Pelvic Floor Dysfunct 1998;9:210-3. PMID: 9795826



17. Withington J, Hirji S, Sahai A. The changing face of urinary continence surgery in England: a perspective from the Hospital Episode Statistics database. BJU Int 2014;114:268-77. PMID: 24512557


18. Abdel-Fattah M, Cooper D, Davidson T, Kilonzo M, Hossain M, Boyers D, et al. Single-incision mini-slings for stress urinary incontinence in women. N Engl J Med 2022;386:1230-43. PMID: 35353961


19. Abdel-fattah M, Ramsay I, Pringle S, Hardwick C, Ali H. Evaluation of transobturator tapes (E-TOT) study: randomised prospective single-blinded study comparing inside-out vs. outside-in transobturator tapes in management of urodynamic stress incontinence: short term outcomes. Eur J Obstet Gynecol Reprod Biol 2010;149:106-11. PMID: 20036048


20. Ogah J, Cody DJ, Rogerson L. Minimally invasive synthetic suburethral sling operations for stress urinary incontinence in women: a short version Cochrane review. Neurourol Urodyn 2011;30:284-91. PMID: 21412819



22. Al-Shaikh G, Syed S, Osman S, Bogis A, Al-Badr A. Pessary use in stress urinary incontinence: a review of advantages, complications, patient satisfaction, and quality of life. Int J Womens Health 2018;10:195-201. PMID: 29713205




23. Thyssen H, Bidmead J, Lose G, Møller Bek K, Dwyer P, Cardozo L. A new intravaginal device for stress incontinence in women. BJU Int 2001;88:889-92. PMID: 11851609



24. Davila GW, Neal D, Horbach N, Peacher J, Doughtie JD, Karram M. A bladder-neck support prosthesis for women with stress and mixed incontinence. Obstet Gynecol 1999;93:938-42. PMID: 10362158


Fig. 1.
A novel incision-free and disposable device: (A) The pelvic floor support disposable pessary-like device. (B) The device’s strap should be outside the vagina for easy removal. (C) The device’s head supports the midportion of the urethra, thereby preventing stress urinary incontinence.
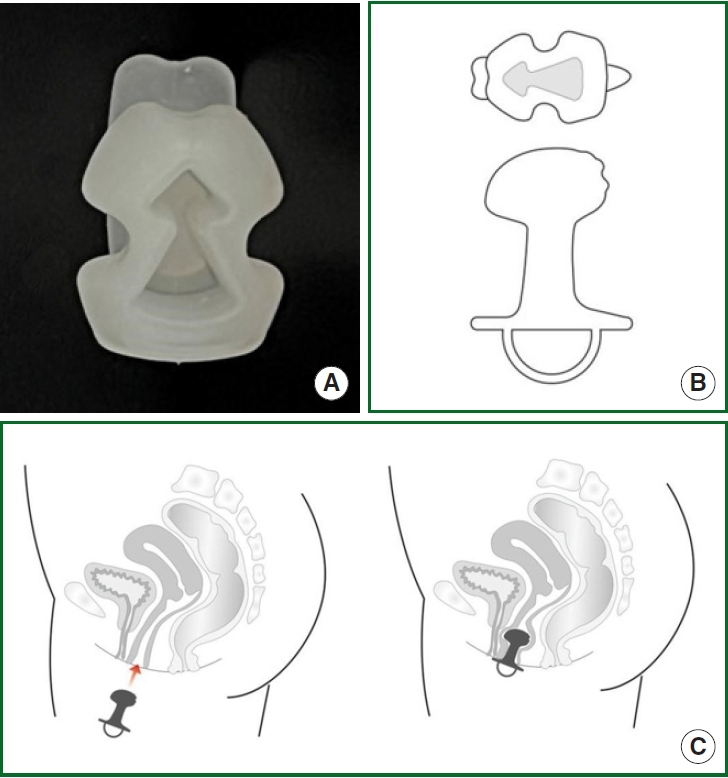
Fig. 3.
Results of the 20-minute pad-weight gain test at baseline and with device use. The percentage of pad-weight gain reduction with device usage is shown by individual subject in decreasing order (n=39). mITT, modified intention-to-treat.
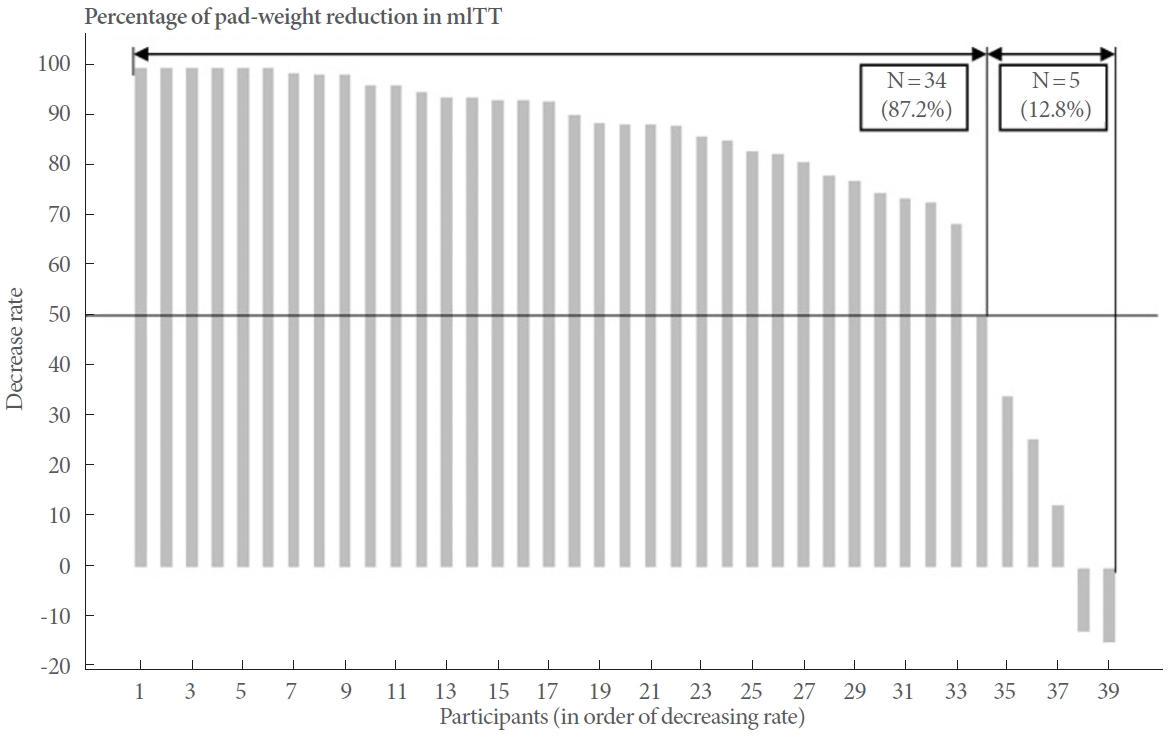
Fig. 4.
Results of patient satisfaction, foreign body sensation, and device compliance population after 1 week of device usage (n=39). (A) Mean±SD patient satisfaction score evaluated using a visual analogue scale (VAS): 6.4±2.6. (B) Mean±SD foreign body sensation evaluated using a 5-point Likert scale: 3.1±1.2. (C) Mean±SD patient compliance calculated by ratio of total usage time (8 hours ×7 days) to expected usage time: 76.6±26.6. SD, standard deviation.

Table 1.
Baseline demographics and clinical characteristics of the study population (n=41)
Table 2.
Results of the 20-minute pad-weight gain test at baseline and visit 3 with device usage
| Pad-weight gain (g) | No. | Mean± SD | Median (range) |
|---|---|---|---|
| At visit 1 (baseline without device use) | 41 | 17.2 ± 33.6 | 6.4 (1.5–172) |
| At visit 3 (with device use) | 39 | 5.3 ± 16.2* | 0.5 (0–67.5) |
Table 3.
Subanalysis of device efficacy, patient satisfaction, foreign body sensation and device compliance according to the baseline demographics and clinical characteristics of the study population
Table 4.
Adverse events