The Metaverse for Healthcare: Trends, Applications, and Future Directions of Digital Therapeutics for Urology
Article information
Abstract
In recent years, the emergence of digital therapeutics as a novel approach to managing conditions has garnered significant attention. This approach involves using evidence-based therapeutic interventions that are facilitated by high-quality software programs to treat, manage, or prevent medical conditions. The incorporation of digital therapeutics into the Metaverse has increased the feasibility of their implementation and application in all areas of medical services. In urology, substantial digital therapeutics are being produced and researched, including mobile apps, bladder devices, pelvic floor muscle trainers, smart toilet systems, mixed reality-guided training and surgery, and training and telemedicine for urological consultations. The purpose of this review article is to provide a comprehensive overview of the current impact of the Metaverse on the field of digital therapeutics and identify its current trends, applications, and future perspectives in the field of urology.
INTRODUCTION
The digital age has opened up a world of possibilities and revolutionized many aspects of healthcare and medical treatment. A particular area of interest is the field of digital therapeutics, which leverages technologies such as artificial intelligence, machine learning (ML), and mobile applications to provide patients with preventive and personalized medical care outside of a traditional clinical setting [1]. Moreover, the recent coronavirus disease 2019 (COVID-19) pandemic has further accelerated the adoption of digital healthcare technologies, including virtual healthcare systems and data analytics, as stakeholders seek to adapt to changing circumstances [2]. In this realm, the Metaverse has become an increasingly important tool for enabling personalized digital therapeutics by connecting health providers and patients with tailored treatment in all areas of medical services. In the field of urology, substantial digital therapeutics, including those related to both benign urological conditions and cancer, are being produced and researched, including mobile apps, bladder devices, pelvic floor muscle trainers, smart toilet systems, mixed reality-guided surgery, and telemedicine for urological consultations.
The review paper provides an overview of how the Metaverse is currently being used in the field of digital therapeutics within the context of urinary treatments. It also identifies current trends and possible future developments, taking into account current achievements and remaining challenges by exploring the current applications of digital therapeutics in urology.
CONCEPTS OF DIGITAL THERAPEUTICS IN THE METAVERSE
Definition of Digital Therapeutics
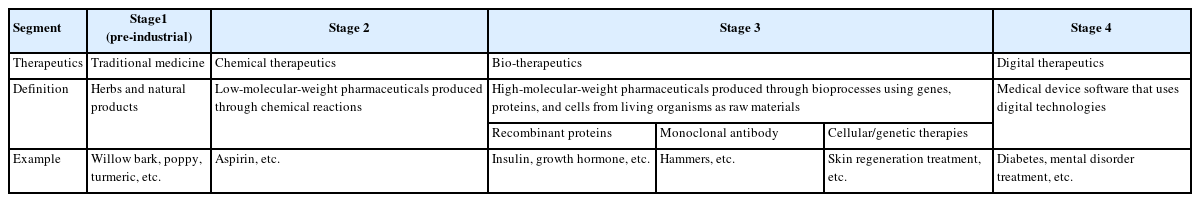
The COVID-19 pandemic has brought about a significant transformation in the healthcare landscape, particularly in terms of its delivery, demand, payment, and regulations. As a result, the digital therapeutics industry has emerged as a promising and efficient solution to address these changes [3]. Digital therapeutics refer to evidence-based therapeutic interventions that utilize software programs to prevent, manage, and treat physical, mental, and behavioral health conditions. As shown in Table 1, digital therapeutics have evolved through several stages and have been receiving an increasing amount of interest as more clinical studies have been conducted to evaluate the potential beneficial effects and safety of these digital interventions [4,5].
Digital therapeutics stand apart from traditional pharmaceuticals in several ways. First, as software without physical form, digital therapeutics employ cognitive behavioral therapy to specifically target the brain and nerves, thereby reducing the likelihood of toxicity and adverse effects [6]. Second, compared to the development of new drugs, digital therapeutics require less time and money for research and development and licensing, which is expected to reduce medical costs [7]. Third, digital therapeutics have the potential to bridge significant care gaps created by shortages of specialized health providers and geographic barriers to accessing physical healthcare systems. They can also provide patients with personalized care quickly, with high accessibility and with less stigma and privacy [8].
There are 3 main therapeutic areas based on treatment modalities. Cognitive behavioral therapy digital therapies are effective in treating central nervous system disorders such as sleep disorders, depression, anxiety, posttraumatic stress disorder, alcohol and drug addiction, pain relief, and panic disorders. This area is relatively active, accounting for one-third of all digital therapeutics development [9,10]. Products for systemic diseases (e.g., diabetes, cancer, and hypertension) where lifestyle improvement has a significant effect, and for diseases where managing the prognosis of seriously ill patients is important, apply a lifestyle modification approach [11]. Digital therapies for medication management are used for diseases that require longterm, regular medication use, such as asthma, chronic obstructive pulmonary disease, and schizophrenia. Additionally, digital therapies are being developed for amblyopia, neurological damage caused by stroke and traumatic injury, and attentiondeficit hyperactivity disorder, utilizing neuro-rehabilitation therapy [9,12].
The Metaverse and its Impact on Digital Therapeutics
The incorporation of digital therapeutics into the Metaverse has been expected to lead to a paradigm shift by increasing the feasibility of their implementation and application [2,13,14] ranging from medical staff training to surgical navigation tools. An example is furnished by digital twins, which are virtual models or simulations of any object, process, or system created using real-world data and augmented reality (AR) and virtual reality (VR)-enabled immersive experiences that allow data collection, analysis, and prediction, collecting and integrating massive amounts of patient data to personalize treatments and track disease progression [15]. The goal is to generate a virtual digital twin in the Metaverse-based on a patient’s medical big data to predict the effectiveness of drug treatment or determine the optimal surgical approach as part of a personalized precision medicine strategy [2].
In its recent report “Metaverse in Healthcare - Global Industry Analysis Outlook and Forecast 2022–2030,” Prescience Research, a strategic market analysis firm based in Canada and India, found that the Metaverse is becoming increasingly important to the healthcare industry. As shown in Fig. 1, the global market size of the Metaverse in healthcare was estimated at United States dollar (USD) 8.9 billion in 2022. It is expected to hit around USD 72.10 billion by 2030 and is poised to grow at a compound annual growth rate of 29.89% from 2022 to 2030 [16].
However, a direct medical model, where the Metaverse is at the center of direct therapeutic effects, is still in the exploratory stage. Park Chul-Ki, chairman of the Medical Metaverse Research Association and a Professor of Neurosurgery at Seoul National University, stated that “the medical practice carried out in the virtual world must be synchronized with reality.” In other words, the creation of a new medical order requires a system that facilitates communication between medical staff and patients, as well as between educators and trainees, rather than simply experiencing VR in the medical Metaverse [17]. Chengoden et al. [14] also mentioned that the adaptation of the Metaverse for healthcare faces challenges relating to patient data security, privacy protection, the high cost of technology, and legal and regulatory concerns.
METAVERSE-BASED APPLICATIONS FOR DIGITAL HEALTHCARE
Telemedicine
Telemedicine is a healthcare delivery model that employs telecommunication technologies to offer medical consultations and services remotely [18]. By using video conferencing, mobile applications, and remote monitoring devices, healthcare providers can diagnose and treat patients in real time, reducing the need for physical visits and enabling patients to receive medical care from their own homes. The versatility of telemedicine renders it suitable for a broad spectrum of medical services, including primary care, mental health, and specialist consultations [19].
Telemedicine is becoming increasingly widely adopted, with the aid of the growing use of digital twins in healthcare. Possik et al. [20] proposed a distributed digital twin implementation of a hemodialysis unit designed to help prevent the spread of the Omicron COVID-19 variant and other infectious diseases. In the system, they used an agent-based discrete event simulator together with a VR environment in order to provide an immersive experience for medical staff that incorporated a platform showing predictive analytics during a simulation run. Another example is illustrated in Fig. 2. Chung-Ang University Gwangmyong Hospital in South Korea has utilized digital twin and Metaverse technologies to create a virtual hospital called “Metaversepital,” allowing users to undergo medical treatment and consultations without needing to physically visit the hospital [21].
Medical Education and Training
The Metaverse technology has the potential to transform medical education by providing an immersive and interactive learning experience that can be personalized to individual needs. It can facilitate collaboration among peers and educators in a 3-dimensional (3D) environment that simulates the classroom setting, enable visualization of virtual 3D structures, improve mentor-mentee interactions, promote self-directed learning, and foster the development of teamwork skills [22]. Although still in the research phase, the use of Metaverse technology has shown promising results in surgical simulations, conferences, awareness and research programs. As shown in Fig. 3, medical Metaverse solutions such as MDBOX aim to provide standardized education regardless of time and location by offering immersive anatomy education through precise anatomical reconstructions in a VR space. Fig. 4 illustrates the MediBase solution, which aims to develop medical simulations for hands-on training in first aid, personal protective equipment, nervous system assessment, and medication administration in a Metaverse environment.

Metaverse medical education product. (A) Virtual reality mode MDBOX image. (B) screen-touch mode MDBOX image for anatomy education tool from MEDICAL IP homepage (https://medicalip.com/MDBOX/).

Metaverse medical simulation of neurological assessments image from NewBase homepage (https://www.newbase.kr/).
Aided Therapy
The Metaverse shows promise for digital therapeutics and offers innovative modes of treatment, particularly in mental health. Its virtual space allows for continuity between virtual and reallife experiences, making it possible for therapeutic effects in the virtual environment to translate into reality. VR also offers unique and controllable situations, making it a suitable option for cognitive behavioral therapy to treat various mental health disorders including anxiety, fear, addiction, and stress. For instance, gameChange, a VR-based Metaverse program (Fig. 5), provides psychotherapy services for psychiatric patients, including those with severe agoraphobia and anxiety among people with psychosis. Freeman et al. [23] investigated the VR therapy of gameChange and concluded that the automated VR therapy is an effective and feasible intervention because the patients who received VR therapy showed greater improvements in anxiety and depression symptoms, quality of life, and social functioning than those who received usual care.
DIGITAL THERAPEUTICS IN UROLOGY
Mobile Apps
With increasing smartphone availability, mobile health apps are a growing field that offers new possibilities for delivering health services. From bladder diaries to apps that find the nearest restroom to videos that remind users how and when to do Kegels, more than 172 apps are eligible in the Apple App Store and Google Play Store. A review of available apps found that most urological apps are geared toward the patient and provide information and services to improve the understanding and treatment of different diseases [24,25]. Devoe et al. [26] evaluated the usability and acceptability of an Android smartphone mobile app designed to help participants learn about overactive bladder symptom management through tracking and selfmanagement. The app included medication reminders, Kegel and bladder training exercises, and monthly, 3-day symptom journals. Another study explored the feasibility of a smartphone app to assess the natural course and management of urinary tract infections (UTIs) and it highlighted that most participants experienced symptom improvement within a week of starting treatment [27].
Dfree is a wearable device for toilet timing prediction to monitor bladder fullness that provides notifications when it is time to use the restroom (Fig. 6). Several studies have demonstrated that using Dfree helped patients with bladder dysfunction, managed their symptoms, improved their quality of life, and increased their overall satisfaction with their care [28]. The device was also found to be easy to use and helped reduce the stigma associated with wearing bulky incontinence products. Dfree and urological mobile apps have been proven to be promising digital therapeutics that offer a noninvasive and convenient approach to managing bladder control issues.
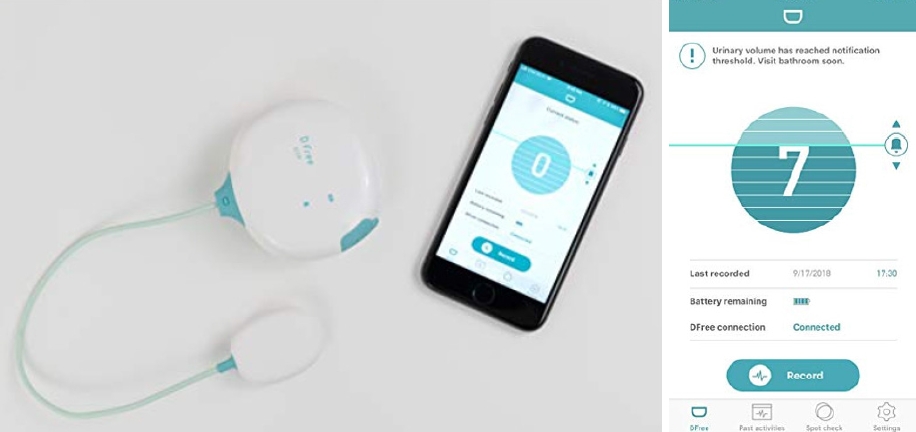
Dfree device and its mobile app image from the Dfree homepage (https://www.dfreeus.biz/).
Pelvic Floor Muscle Training
Pelvic floor muscle training is the first-line treatment for stress urinary incontinence, but cure rates are low. Many women find it difficult to distinguish between a “lift” and “squeeze” and to perform a Valsalva maneuver, or engage in other incorrect pelvic floor muscle motions. Therefore, digital therapeutic devices have been designed and produced to help women strengthen their pelvic floor muscles, which can help to reduce symptoms of urinary incontinence. Motion-based biofeedback devices (Fig. 7), including the leva Pelvic Health System, the Elvie Trainer, and Magic Kegel, are designed to be inserted into the vagina and communicate wirelessly with an app downloaded to the patient’s smartphone. Accelerometers or motion sensors along the length of the device provide visual feedback to the patient about pelvic floor muscle action. These mobile home pelvic floor muscle trainers have been clinically tested and shown to be effective in improving symptoms of urinary incontinence and quality of life in women who use them regularly [29,30]. Artymuk and Khapacheva [31] suggested that a device-assisted pelvic floor muscle exercise program with Magic Kegel can be an effective and more satisfactory approach to managing pelvic floor dysfunction after delivery. It can be inferred from these findings that digital therapeutic devices have the potential to offer an efficient and user-friendly treatment option for women with urinary incontinence.
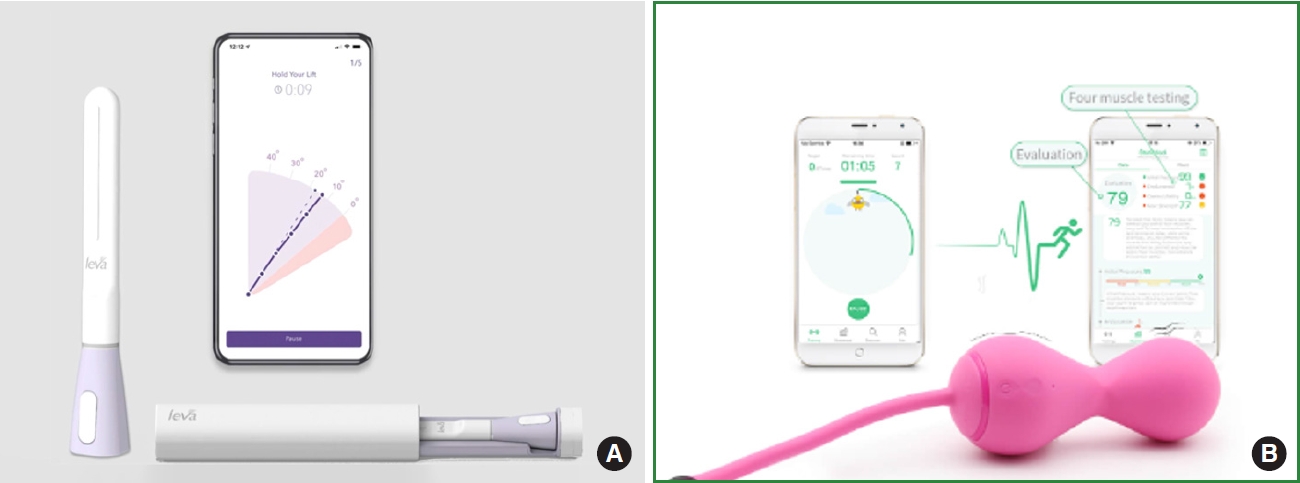
Mobile home pelvic floor muscle trainer. (A) The leva product image from leva pelvic health system homage (https://www.levatherapy.com/). (B) Magic Kegel Master image from Magic Motion homepage (https://www.magicsmotion.com/).
Smart Toilet Systems
A smart toilet system is a technological innovation that integrates various sensors and devices into a traditional toilet to monitor and analyze a user’s urine and feces. Bhatia et al. [32] proposed a smart toilet system that utilizes Internet of Things technology to predict UTIs at home. The system integrated various sensors to monitor key biomarkers in urine and used ML algorithms to predict the likelihood of a UTI. Fig. 8 illustrates the major toilet products that offer a range of features and technologies that can help individuals with urological issues to maintain better hygiene and comfort, and reduce the risk of infection. Oh et al. [33] introduced the major international smart toilet service products and their recent developments and Wu and Sun [34] proposed a design approach to improve user experience and satisfaction with smart toilets by utilizing the peak-end rule. These recent studies show the potential of smart toilet systems to revolutionize the diagnosis and management of various urological conditions and offer a noninvasive and convenient method for monitoring patients with chronic urological conditions, such as interstitial cystitis or bladder cancer [35,36].

Smart toilet products. (A) Electric Bidet DL-EH10 image from Panasonic homepage (https://www.panasonic.com/my/consumer/home-appliance/bidet/electric-bidet/dl-eh10se-w.html/). (B) TOTO smart toilet catalog image from Toto homepage (https://kr.toto.com/49/service/download/).
Mixed Reality-Guided Training and Surgery
Recent advancements in the Metaverse technology have led to its growing significance in the field of urological surgery, including surgical training. The concept of image-guided surgery and intervention has been extensively deliberated [37,38], and the efficacy of AR visualization for image-guided surgery has been confirmed through the use of 3D-printed phantoms [39,40]. By projecting a 3D virtual model onto a patient’s body, AR technology allows surgeons to retrieve patient information in a hands-free manner. Moreover, the use of AR technology coupled with the patient’s anatomy permits the real-time visualization of tumor characteristics and 3D anatomy, which are specific to each individual patient, improving the safety and efficacy of surgical procedures [41].
Robotic surgery has become a mainstay in certain urological diseases, and the robotic approach has become more widely utilized for ureteral reconstruction [42]. Fluorescence-guided surgery, 3D imaging technologies, and other innovative devices are rapidly revolutionizing the field of urology, providing surgeons with powerful tools for a more complete understanding of patient-specific anatomy [43]. In the field of pediatric urology, AR devices have been increasingly adopted for a more realistic understanding of normal and abnormal anatomy, providing valuable insights to deliver customized treatments in real time [44]. As shown in Fig. 9, the Minimally Invasive Surgery Centre (CCMIJU) in Spain uses mixed reality technology, by means of Microsoft’s HoloLens glasses, to enable the creation of new and more realistic scenarios for medical training and improve surgical results [45]. The CCMIJU’s team led by Dr. Sanchez-Margallo et al. [46] proposed that mixed reality technology can provide improved visualization and spatial understanding of anatomical structures, as well as haptic feedback, which could be particularly useful for urological procedures that involve delicate manipulations of tissues and organs.
Telemedicine Platforms
Telemedicine has emerged as a promising approach for transforming the delivery of urological consultations. It has been observed to significantly reduce both time and costs while yielding satisfactory outcomes for patients and clinicians alike; for instance, Margolin et al. found telemedicine to be as effective as in-person visits for urological cancer care and counseling [47,48]. In particular, telemedicine has presented an opportunity to address sexual health-related urological concerns in a patient-centered and comfortable manner [49].
According to a KPMG survey conducted by HIMSS Analytics, the usage of video-based telemedicine services and remote patient monitoring stands at 31% and 34%, respectively, among healthcare organizations [50]. American Well is one such vendor that provides telehealth visits by video and phone, with the majority being video-based, and it has started on-demand virtual care services with Thomas Jefferson University Hospitals (Fig. 10). Patients can log in and schedule an appointment with a healthcare provider or join a virtual waiting room through a secure video connection, where they can discuss their symptoms, receive a diagnosis, and receive treatment recommendation. These virtual visits provide a variety of helpful services, including behavioral health, neurology, postdischarge and urology.
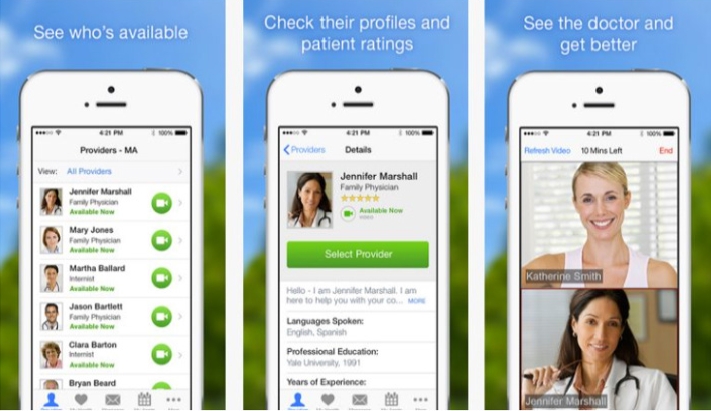
JeffConnect: on-demand virtual care app image from its website (https://www.jeffconnect.org/).
The MUTU system is another example of a telemedicine service platform designed to support postpartum women in recovering and strengthening their pelvic floor muscles. As shown in Fig. 11, this program provides a range of online resources, including customized workouts and coaching, to help women improve their pelvic health and regain confidence in their bodies.
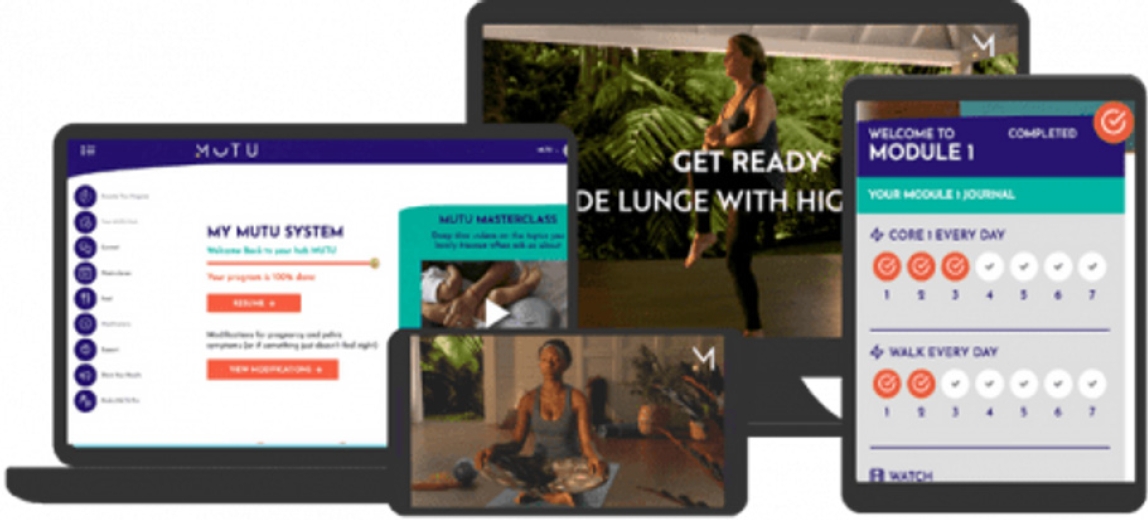
Screenshots of MUTU System image from its website (https://mutusystem.com/en-us/).
CONCLUSIONS
This paper presents the applications of technology-based interventions such as mobile apps, wearable devices, online platforms, and mixed reality technologies for urinary symptoms and prevention as a form of Metaverse-based digital therapeutics. Some domestic and international cases and research studies were also reviewed to demonstrate the accountability and implications of these therapies. The paper introduced examples of digital therapeutics in urology including bladder diaries, pelvic floor muscle exercise trainers, smart toilet systems, mixed reality-guided surgery, telemedicine for urological consultations, and VR-based interventions for pain management and rehabilitation. Digital therapeutics have also shown the potential to improve patient outcomes, reduce healthcare costs, and increase patient satisfaction. While the use of digital therapeutics in urology is still in its early stages, it can be an effective addition to traditional treatment methods and may provide patients with more options for their various urological conditions. In order for digital therapeutics for urinary disease to be integrated into clinical practice guidelines, more clinical evidence needs to be gathered for physicians to have confidence in the accuracy of the data collected by the sensors, which will require the development of professionally trained medical virtualists. Additionally, the usage process must be clearly defined, and the discomfort associated with wearable devices must also be improved to increase patient compliance. In conclusion, additional investigations and advances are required to fully maximize the potential of digital therapeutics in various areas of medical treatment, including the field of urology, in the era of the Metaverse.
Notes
Grant/Fund Support
This research was supported by Basic Science Research Program through the National Research Foundation of Korea (NRF) funded by the Ministry of Education (NRF-2022R1F1A1066602).
Conflict of Interest
No potential conflict of interest relevant to this article was reported.
AUTHOR CONTRIBUTION STATEMENT
· Conceptualization: JYK
· Data curation: EJK
· Formal analysis: EJK
· Funding acquisition: JYK
· Methodology: EJK, JYK
· Project administration: JYK
· Visualization: EJK, JYK
· Writing - original draft: EJK
· Writing - review & editing: EJK, JYK