Meta-Analysis of the Efficacy and Safety of Mirabegron Add-On Therapy to Solifenacin for Overactive Bladder
Article information
Abstract
Purpose
We performed a meta-analysis to evaluate the efficacy and safety of mirabegron add-on therapy to solifenacin for patients with overactive bladder (OAB).
Methods
We conducted a systematic literature review to identify all randomized, double-blind, controlled trials (RCTs) of this combination (mirabegron and solifenacin) for OAB. Embase, MEDLINE, and the Cochrane Central Register of Controlled Trials were searched. A manual search was also performed to investigate relevant references from the retrieved studies.
Results
Four publications describing 5 RCTs that compared combination therapy with solifenacin, including a total of 3,309 patients, were analyzed. The mean number of micturitions per 24 hours (mean difference [MD], -0.45; 95% confidence interval [CI], -0.65 to -0.26; P<0.00001), number of episodes of incontinence per 24 hours (MD, -0.71; 95% CI, -0.14 to -0.02; P=0.04), volume voided per micturition, and number of urgency episodes per 24 hours demonstrated that combination therapy was more effective than solifenacin therapy alone. Safety assessments, including common treatment-emergent adverse events (odds ratio, 1.09; 95% CI, 0.95–1.27; P=0.23) and discontinuations due to adverse events (P=0.30), demonstrated that the combination therapy was well tolerated.
Conclusions
This meta-analysis suggests that mirabegron therapy as an add-on to solifenacin provides a satisfactory therapeutic effect for OAB symptoms with a low occurrence of side effects.
INTRODUCTION
Overactive bladder (OAB) is characterized by symptoms of urinary urgency, frequency, and nocturia with or without urgency incontinence in the absence of a lower urinary tract infection [1]. OAB is a common multifactorial health disorder that is associated with detrimental effects on quality of life and a considerable economic burden [2]. The prevalence of OAB is high, with 12%–16% of adults in Europe, the United States, and Asia affected by this symptomatic syndrome [3].
Antimuscarinic agents are the mainstay of oral pharmacotherapy for OAB, but long-term treatment is limited by their insufficient efficacy and antimuscarinic agent-associated adverse events (AEs). In clinical practice, antimuscarinics are often initially prescribed; however, increasing the dose may exacerbate antimuscarinic AEs, such as constipation and dry mouth, and result in treatment discontinuation [4]. The efficacy of β3-adrenergics, which are associated with a new safety profile that differs from that of antimuscarinics, has been shown [5]. Mirabegron is a selective β3-adrenoceptor (AR) agonist [6] that is the drug of first choice for OAB. Given that β3-adrenergics and anticholinergics have distinct mechanisms of action, the combination of both drugs is a possible option and has been tested in several clinical trials [7,8].
We performed a meta-analysis to evaluate the safety and efficacy of the combination of solifenacin (5 or 10 mg) plus mirabegron (50 mg) compared with solifenacin (5 or 10 mg) monotherapy (the most widely used doses in clinical practice) for OAB treatment.
MATERIALS AND METHODS
Search Strategy
A systematic search of the literature was undertaken using Embase (1993 to May 2017), MEDLINE (1966 to May 2017), and the Cochrane Central Register of Controlled Trials to retrieve published randomized controlled trials (RCTs) investigating the use of mirabegron add-on therapy to solifenacin for OAB. We searched the database using combinations of the following terms: “mirabegron, solifenacin, OAB, and RCT.” Additionally, the references of the retrieved articles were screened.
Inclusion Criteria
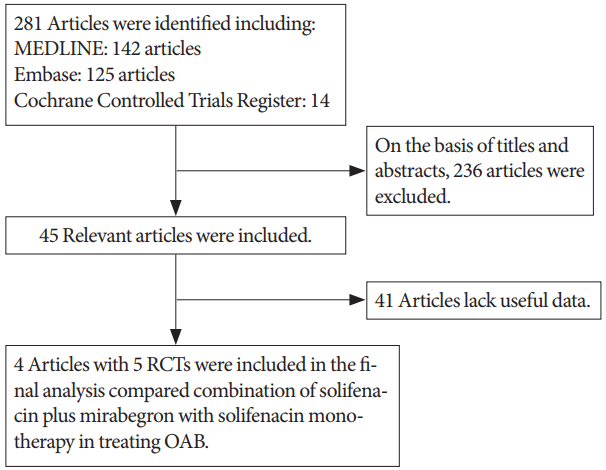
The following criteria were used to select the RCTs: (1) mirabegron add-on therapy to solifenacin was analyzed in the study, (2) the full text of the selected study was accessible, and (3) accurate data were provided and could be analyzed (including the values of each parameter that was analyzed and the total number of subjects). When the same group of researchers investigated a certain subject group in multiple experiments, each study was included. Additionally, the most recently published study was included in the meta-analysis if an identical study was published in distinct journals or at a different time point. The flowchart in Fig. 1 depicts the selection process.
Quality Assessment
The Jadad scale was used to determine the quality of the retrieved RCTs [9]. The methodological quality of each study was assessed according to the patient allocation method, blinding method, concealment of allocation procedures, and data loss due to discontinuation. Then, the studies were qualitatively classified according to the guidelines presented in the Cochrane Handbook for Systematic Reviews of Interventions version 5.1.0 [10]. Each study was assigned and rated according to the following quality categories: A, the study had a low risk of bias if all quality criteria were adequately fulfilled; B, the study had a moderate risk of bias if one or more quality criteria were merely partially met or were ambiguous; or C, the study had a high risk of bias if one or more of the criteria were barely met or were not included. Differences were settled by discussion between the authors.
Data Extraction
The following usable information was extracted from each study: (1) first author’s name; (2) country of the study; (3) sample size; (4) year of publication; (5) therapy for the patients; and (6) data on the mean number of micturitions per 24 hours, mean number of episodes of incontinence per 24 hours, mean volume voided per micturition, mean number of urgency episodes per 24 hours, common treatment-emergent adverse events (TEAEs), and discontinuations due to AEs.
Statistical Analysis and Meta-Analysis
The meta-analysis was conducted using RevMan version 5.1.0. (Cochrane Collaboration, Oxford, UK) [10]. Differences between the entry and endpoint of the study were evaluated according to the changes in the mean number of micturitions per 24 hours, mean number of episodes of incontinence per 24 hours, mean volume voided per micturition, mean number of urgency episodes per 24 hours, discontinuations due to AEs, and common TEAEs. Fixed-effects and random-effects models were used to assess the mean difference (MD) for continuous data and the odds ratio (OR) for dichotomous results pooled across studies with the corresponding 95% confidence interval [CI] [11]. A study was considered homogeneous only when the analysis showed a P-value of >0.05, in which case a fixed-effects model was chosen for the meta-analysis; otherwise, a random-effects model was considered more appropriate.
RESULTS
Characteristics of the Individual Studies
The database search yielded 281 articles. A total of 236 studies were removed after reviewing the titles and abstracts of the articles according to the inclusion and exclusion criteria described above. A total of 41 of the remaining 45 articles were excluded due to a lack of useful data, and as a result, 4 articles describing 5 RCTs [12-16] that compared the combination of solifenacin (5 or 10 mg) plus mirabegron (50 mg) to solifenacin (5 or 10 mg) monotherapy were included in the analysis (Fig. 1). Table 1 presents relevant information about the articles.
Quality of the Individual Studies
All 5 RCTs were double-blinded, and all the articles elaborated on their randomization processes. All the included RCTs conducted a power calculation to determine the optimal sample size (Table 2). The level of quality of each study was A (Table 2). The funnel plot generated to provide a qualitative estimation of the publication bias of the studies suggested no evidence of bias (Fig. 2).
Efficacy
Mean number of micturitions per 24 hours
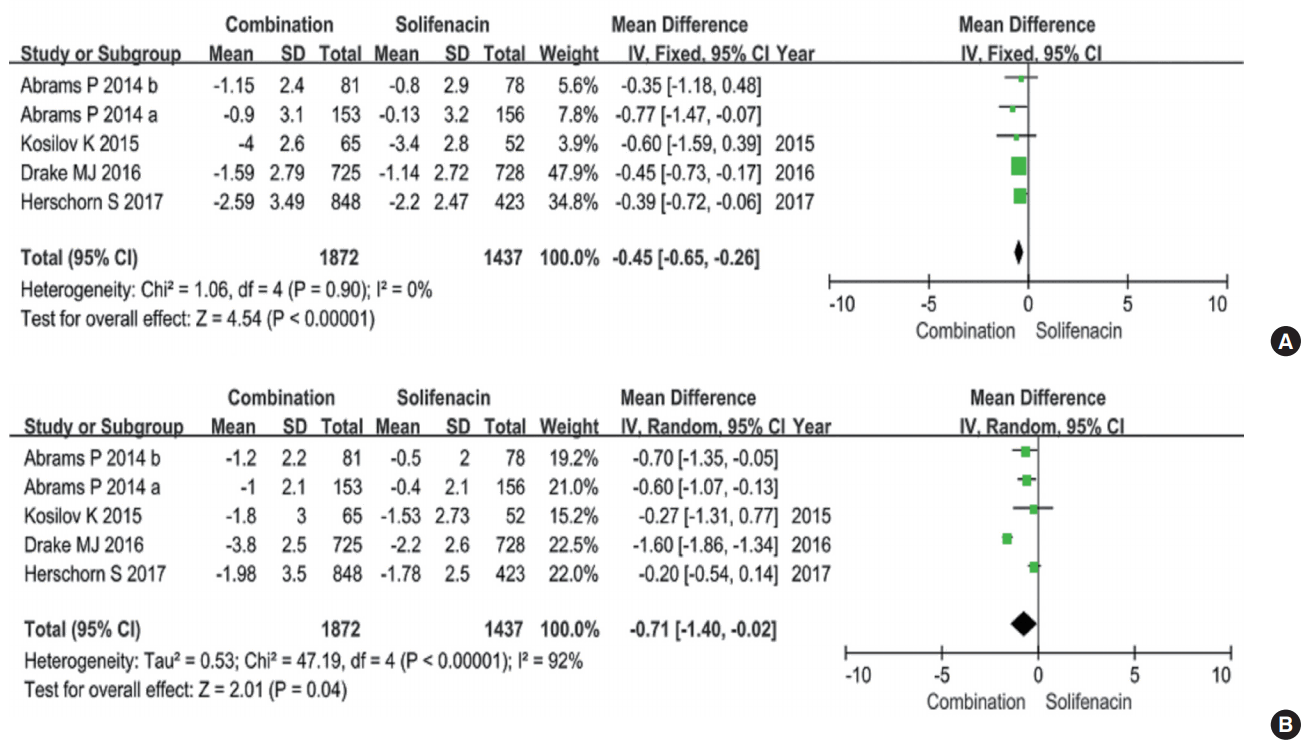
Five RCTs included data on the mean number of micturitions per 24 hours, for a cohort of 3,309 participants (1,872 in the combination group and 1,437 in the solifenacin group) (Fig. 3). The fixed-effects estimate of the MD was -0.45, and the 95% CI was -0.65 to -0.26 (P<0.00001). This result suggests that mirabegron add-on therapy to solifenacin showed superior efficacy in reducing the mean number of micturitions per 24 hours compared with solifenacin alone.
Mean number of episodes of incontinence per 24 hours
Five RCTs included data on the episodes of incontinence per 24 hours for a total of 3,309 participants (1,872 in the combination group and 1,437 in the solifenacin group) (Fig. 3). The random-effects estimate of the MD was -0.71, and the 95% CI was -1.40 to -0.02 (P=0.04). This result indicates that the combination group experienced greater decreases in episodes of incontinence per 24 hours.
Mean volume voided per micturition
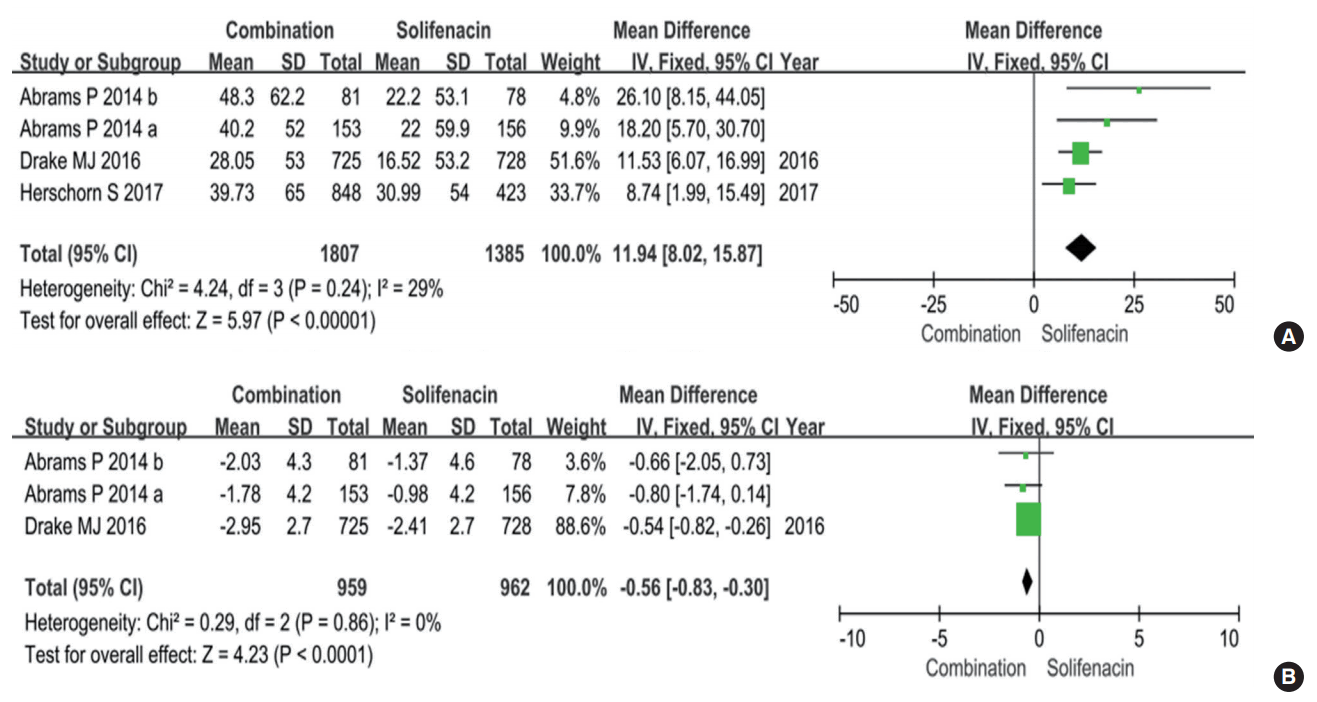
Four RCTs with a total of 3,192 participants (1,807 in the combination group and 1,385 in the solifenacin group) (Fig. 4) were identified. The fixed-effects estimate of the MD was 11.94, and the 95% CI was 8.02 to 15.87 (P<0.00001). This result suggests that the combination group experienced greater increases in the mean volume voided per micturition.
Mean number of urgency episodes per 24 hours
Three RCTs with a total of 1,921 participants (959 in the combination of solifenacin plus mirabegron group and 962 in the solifenacin group) (Fig. 4) were identified. The fixed-effects estimate of the MD was -0.56, and the 95% CI was -0.83 to -0.30 (P<0.0001). This result suggests that mirabegron add-on therapy to solifenacin successfully reduced the mean number of urgency episodes per 24 hours.
Safety
Treatment-emergent adverse events
Five RCTs with a total of 3,309 participants (1,872 in the combination group and 1,437 in the solifenacin group) included TEAE data (Fig. 5). The OR was 1.09, and the 95% CI was 0.95 to 1.27 (P=0.23). This result indicates that the groups were similar in terms of the incidence of TEAEs.
Discontinuation due to AEs
Five RCTs with a total of 3,309 participants (1,872 in the combination group and 1,437 in the solifenacin group) reported discontinuation due to AEs (Fig. 5). The pooled estimate of the OR was 1.33, and the 95% CI was 0.78 to 2.27 (P=0.30). No apparent differences were found between the combination group and the solifenacin-only group in terms of discontinuation due to AEs.
Urinary retention, dry mouth, and blurred vision
Three RCTs, representing 2,841 participants (1,638 in the combination group and 1,203 in the solifenacin group), included data on urinary retention. The pooled estimate of the OR was 1.74, and the 95% CI was 0.55 to 5.45 (P=0.34). Five RCTs included data on dry mouth (OR, 0.99; 95% CI, 0.73–1.33; P=0.93), and 4 RCTs included data on blurred vision (OR, 1.80; 95% CI, 0.52–6.18; P=0.35). These results suggest that there were no apparent differences between the combination group and the solifenacin-only group in terms of the incidence of urinary retention, dry mouth, and blurred vision.
DISCUSSION
OAB is one of the most frequent lower urinary tract symptoms (LUTS) in both genders and is associated with significant bothersome symptoms and a poorer quality of life [17]. In many cases, no underlying cause is found, and the case of OAB is considered idiopathic [18]. Pharmacological therapy is widely used for OAB treatment. The 2 main classes of drugs used are antimuscarinics and the newer β3-AR agonists [19]. Combining 2 oral pharmacotherapies with distinct modes of action and proven efficacy may improve OAB symptoms without exacerbating the burden of anticholinergic or β3-AR agonists, which can obviate the need for dose escalation or more invasive interventions [20].
This systematic review and quantitative meta-analysis summarized the evidence from RCTs regarding the efficacy and safety of mirabegron (50 mg per day) add-on therapy to solifenacin (5 or 10 mg per day) for OAB treatment. Our study demonstrated that the combination therapy was superior to solifenacin alone (5 or 10 mg per day) in improving the mean number of micturitions per 24 hours, the mean number of episodes of incontinence per 24 hours, the mean volume voided per micturition, and the mean number of urgency episodes per 24 hours. Two RCTs [13,14] evaluating the mean number of nocturia episodes, mean number of pads per 24 hours, and the Patient Perception of Bladder Condition score showed that adding mirabegron therapy to solifenacin was superior to solifenacin alone for improving OAB symptoms. One RCT [15] demonstrated that the postvoid residual bladder capacity, detrusor compliance, and maximum bladder capacity values significantly changed in the combination group. Overall, the combination therapy resulted in more pronounced improvements in multiple parameters. The findings indicate that combination therapy may be more useful than monotherapy for patients seeking additional symptomatic improvement.
Yamaguchi et al. [21] reported the results of the MILAI study, which was an open-label phase IV trial that demonstrated the effects of mirabegron as an add-on therapy in patients in whom OAB was treated with solifenacin. The authors discovered that the addition of mirabegron to solifenacin resulted in only mild to moderate AEs and had promising results in terms of efficacy. Imamura et al. [22] found that the different mechanisms of action of mirabegron and solifenacin were synergistic in inhibiting cold stress-induced detrusor overactivity in spontaneously hypertensive rats. Therefore, the combination of mirabegron and solifenacin offered significant improvements over single-drug treatment and lacked serious side effects in patients with cold stress-exacerbated LUTS.
When urine is stored, the binding of acetylcholine in the bladder activates afferent nerves to the muscarinic receptors (MRs) [23]. MR antagonists can effectively suppress the activation of the afferent nerves by blocking MRs. Additionally, MR antagonists may desensitize the bladder afferent nerves [24]. In contrast, β3-AR agonists stimulate the release of nitric monoxide (NO) by the urothelium [25] by binding to receptors within the urothelium. NO suppresses the activation of the afferent nerves, and β3-AR activation has an inhibitory effect on bladder afferent activity. Moreover, the combination of antimuscarinic and β3-AR agonist agents was found to inhibit part of the Rho kinase pathway in vitro [26]. As a result, the combination of mirabegron and solifenacin may effectively improve bladder function during the storage phase by inhibiting afferent nerve activation.
The safety data included in this meta-analysis suggest that the combination of mirabegron and solifenacin is well tolerated. Measures of adverse reactions, such as discontinuations due to AEs and common TEAEs, were similar in the combination group and the solifenacin-only group. This result demonstrates the safety of mirabegron add-on therapy to solifenacin for OAB treatment. Dry mouth, which was the most frequently reported AE with antimuscarinics [27] and a common reason for treatment discontinuation [4], did not show a different pattern of incidence in the combination versus solifenacin-only groups. The vital signs, electrocardiogram parameters, and postvoid residual volume in the combination group showed no synergistic effects beyond those known from either monotherapy. Therefore, mirabegron (50 mg per day) add-on therapy to solifenacin (5 or 10 mg per day) seems to offer a good balance between side effects and efficacy.
This meta-analysis included only double-blind RCTs. The quality of the individual studies in the meta-analysis was high based on the quality assessment scale that we developed. Nevertheless, few studies were included. The long-term safety, efficacy, and persistence of combination therapy cannot be extrapolated from this article, and the present analysis excluded data from unpublished studies. These factors may contribute to bias. Although the combination of either 5 mg or 10 mg of solifenacin with 50 mg of mirabegron was found to be effective, the impacts of add-on treatment over monotherapy according to solifenacin dosage (5 mg vs. 10 mg) might be different. In this regard, it would be preferable to show that there was no difference in the efficacy and safety according to the solifenacin dosage. However, such a comparison could not be conducted because of small number of RCTs that were included. More high-quality trials with larger sample sizes should further investigate the efficacy and safety of mirabegron add-on therapy to solifenacin for OAB. Furthermore, cost is an important factor, particularly for older adults who may have high out-of-pocket costs associated with these drugs.
This meta-analysis indicates that mirabegron add-on therapy to solifenacin provides a satisfactory therapeutic effect for OAB symptoms without increasing the risk of side effects.
HIGHLIGHTS
- We performed a meta-analysis to evaluate the efficacy and safety of mirabegron add-on therapy to solifenacin for patients with OAB.
- This meta-analysis suggests that mirabegron therapy as an add-on to solifenacin provides a satisfactory therapeutic effect for OAB symptoms with a low occurrence of side effects.
Notes
Conflict of Interest
No potential conflict of interest relevant to this article was reported.