 |
 |


- Search
| Int Neurourol J > Volume 21(3); 2017 > Article |
|
ABSTRACT
Purpose
This study aimed to investigate potential biomarkers for the diagnosis of overactive bladder (OAB).
Methods
A total of 219 subjects were enrolled and divided into 2 groups: OAB subjects (n=189) and controls without OAB symptoms (n=30). Three-day voiding diaries and questionnaires were collected, and urinary levels of nerve growth factor (NGF), prostaglandin E2, and adenosine triphosphate were measured and normalized to urine creatinine (Cr). Baseline characteristics and urinary levels of markers were analyzed. A receiver-operator characteristic (ROC) curve was used to analyze the diagnostic performance of urinary markers. Urinary levels of markers according to subgroup and pathogenesis of OAB were evaluated. Correlation analyses were used to analyze the relationship between urinary levels of markers and voiding diary parameters and questionnaires.
Results
There was no difference between the 2 groups with regards to age, sex ratio, or urine Cr (P>0.05). The urinary levels of NGF/Cr were higher in OAB subjects than in controls (P<0.001). Urinary NGF/Cr was a sensitive biomarker for discriminating OAB patients (area under the curve=0.741; 95% confidence interval, 0.62–0.79; P=0.001) in the ROC curve. The urinary levels of NGF/Cr were significantly higher in OAB subjects than in controls regardless of subgroup or pathogenesis. Correlation analysis demonstrated urinary urgency was significantly related to urinary NGF/Cr level (correlation coefficient, 0.156). Limitations include a relatively wide variation of urinary markers.
The overall prevalence of overactive bladder (OAB) in Europe is 16.6% in the population over 40 years old (male, 15.6%; female, 16.4%) [1]. The prevalence of OAB tends to increase with age [2,3]. It can interfere with quality of life and social activities [4-6]. The precise pathogenesis of OAB is likely multifactorial and remains to be clarified [7]. There are several substances that have been proposed as biomarkers of OAB, but to our knowledge, studies in the same cohort that have compared these markers are lacking.
Nerve growth factor (NGF) is a small secretory protein that brings about the differentiation and survival of specific target neurons. In the bladder, NGF is produced by smooth muscle and urothelium [8]. Chuang et al. [9] demonstrated in an animal model that NGF leads to induced bladder hypersensitivity, due to the sensitization of afferent nerve pathways without inflammation. Urinary levels of NGF are elevated in OAB patients, and have been proposed as a potential biomarker [10-12].
Prostaglandin E2 (PGE2) in the bladder is produced by muscle and mucosa in the cyclooxygenase pathways, detrusor muscle stretch, nerve stimulation of the bladder, and mucosal injury. This synthesis is initiated by inflammation. Thus, increased levels of PGE2 have also been proposed as an OAB biomarker [13,14].
Adenosine triphosphate (ATP) is released by stretching of the urothelium. ATP has been suggested as a mediator of transducing external stresses of the bladder wall. Uroepithelial cells are considered to be a primary source of ATP in the bladder [15]. In prior studies, release of activated ATP by stretching was enhanced in tissues from OAB patients, leading to its suggestion as yet another biomarker [7,16].
Although NGF, PGE2, and ATP may play important roles as biomarkers as proposed in several studies, OAB treatment based on a biomarker, in comparison to treatment based on a diagnosis made from a careful examination of patient history, is not supported by current literature [17]. Thus, this study investigated the appropriateness of the above-mentioned biomarkers for the diagnosis of OAB.
This study was approved by the Institutional Review Board of our institution (approval number: 2010-05-106), and registered at ClinicalTrials.gov (NCT01515722). Written informed consent was obtained from all subjects. A total of 219 subjects who visited the outpatient clinic from February 2010 to February 2015 were enrolled. The OAB group comprised 189 subjects over 18 years old with a symptom duration of ≥3 months, ≥8 micturitions/24 hours, and ≥2 urgency episodes/24 hours reported in 3-day voiding diary [18]. The control group contained 30 subjects over 18 years old without OAB symptoms with ≤7 micturitions/24 hours and ≤1 urgency episodes/24 hours. The mean urinary sensation scale (USS) score in the 3-day voiding diary was considered as the USS of the patient and urgency was defined as USS ≥3 [19].
Subjects were excluded if they had stress urinary incontinence, hepatic or renal disease, any condition that is a contraindication for anticholinergic treatment, urinary tract infection, interstitial cystitis, hematuria, a history of undergoing prostate or bladder neck surgery due to bladder outlet obstruction, pelvic organ prolapse, bladder or prostate cancer, or chronic constipation. Subjects were also excluded if they used an unstable dosage of any drug with anticholinergic side effects, or expected to start such treatment during the study, were pregnant or nursing, had an indwelling catheter or practiced intermittent self-catheterization, were sexually active females of childbearing potential not using reliable contraception, had ever received any electrostimulation or bladder training, had treatment with any anticholinergic drugs or any drug for OAB within the 14 days before randomization, or expected to start such treatment during the study, had received treatment with potent CYP3A4 inhibitors, or had used any investigational drug within 2 months preceding the start of the study.
All subjects were requested to submit a 3-day voiding diary, and urine samples for measuring NGF, PGE2, ATP, and creatinine (Cr) were collected. Overactive Bladder Questionnaire Short Form (OAB-q SF) symptom bother scale, the health-related quality of life questionnaire (HRQoL), and the Overactive Bladder Symptom Score survey (OABSS) were collected from OAB subjects [20,21].
Urinary NGF, PGE2, and ATP were normalized to urinary Cr, and the baseline characteristics of the controls and OAB subjects were analyzed. The urinary levels of NGF/Cr, PGE2/Cr, and ATP/Cr were measured in both the control and OAB subjects. A receiver-operator characteristic (ROC) curve was used to analyze the diagnostic performance of biomarkers. The urinary levels of NGF/Cr, PGE2/Cr, and ATP/Cr were evaluated according to subgroups (OAB-dry or OAB-wet) and pathogenesis (idiopathic or neurogenic) of OAB. The idiopathic OAB was defined when no identifiable cause for OAB was found. The neurogenic OAB was defined when nervous system conditions including spinal cord injury, stroke, diabetic neuropathy, multiple sclerosis, Parkinson disease, or dementia were noted. Correlations between voiding diary parameters, questionnaires, and levels of urinary markers were analyzed.
Urine samples were immediately put on ice and then centrifuged at 3,000 rpm at 4˚C for 10 minutes. The supernatants were carefully separated into aliquots in 1.5-mL tubes and preserved at -80˚C. Urinary Cr was measured using 3 mL of urine aliquots.
The concentration of urinary NGF was measured by the NGF Emax ImmunoAssay System (Promega, Madison, WI, USA). First, 10-μL anti-NGF polyclonal antibody that was diluted in 10-μL carbonate coating buffer (pH, 9.7) was pipetted into each well for coating 96 well plates. After sealing, the wells were incubated overnight at 4˚C. The wells were washed 3 times with tris-buffered saline with Tween 20 (TBST) washing buffer (20mM Tris-HCl, 150mM NaCl, and 0.05% Tween 20) and incubated with sample buffer and 200 μL 1×buffer for 1 hour at room temperature (RT). An NGF standard and each 100-μL urine sample were added to the wells. After incubation for 6 hours, the wells were washed with TBST 5 times, and then 100 μL secondary antibody (2.5-μL anti-NGF monoclonal antibody that was diluted in 10 mL 1×block and sample buffer) was added to each well. The plates were incubated at 4˚C overnight. After washing each 100 μL well 5 times with TBST washing buffer, 100-μL anti-rat IgG horseradish peroxidase conjugate was added and the wells were then incubated at RT for 2.5 hours. Once again, the wells were washed 5 times with TBST washing buffer, and were then incubated with 100-μL tetramethylbenzidine substrate solution at RT for 10 minutes, and 100 μL of 1N hydrochloric acid was added for termination of the reactions. The amount of NGF was determined by the VersaMax ELISA Microplate Reader (Molecular Devices Inc., Sunnyvale, CA, USA) at 450 nm.
The Prostaglandin E2 Parameter Assay Kit (R&D Systems Inc., Minneapolis, MN, USA) was used for measuring PGE2. Reagents, samples, and standards were prepared according to the manufacturer’s instructions. First, 200-μL calibrator diluent RD5-56 was added to the nonspecific binding wells. Then 150-μL calibrator diluent RD5-56 was added to the zero standard (Bo) wells, and 150 μL of standard, control, or sample was added to the remaining wells. After that, 50-μL primary antibody solution was added to each well and incubated for 1 hour at RT. 50-μL PGE2 conjugate was added to wells and incubated for 2 hours at RT, then aspirated and washed 4 times. Next, 200-μL substrate solution was added to each well, incubated for 30 minutes at RT, while being protected from light. After that, 100-μL stop solution was added to each well and PGE2 levels were measured by the ELISA (enzyme-linked immunosorbent assay) reader.
An Adenosine 5’-triphosphate Bioluminescent Assay Kit (Sigma-Aldrich, St. Louis, MO, USA) was utilized for ATP measurement. Urine samples were diluted with sterile distilled water (DW), dissolving 1mg (2×10-6 mole) in 1-mL sterile DW, aliquoted into 100-μL fractions, and kept at -20˚C. The luciferin-luciferase mixture was added using the ATP Bioluminescence Assay Kit HS II (Roche Applied Science, Indianapolis, IN, USA). A 100-μL sample was added to 900-μL DW to make serial dilutions (2×10-7–2×10-15). Then, 100 μL of ATP Assay Mix stock solution was added to the tube and kept for 3 minutes at RT to allow for hydrolysis of endogenous ATP to diminish background, 15 assays at a time. 100-μL DW was added to 100 μL of the ATP Assay Mix solution, mixed, and then added to the 96 well plate. The blank wells were measured for 5 seconds with a luminometer. The light values from the blanks were excluded from those of the samples to achieve final values. The blanks for the ATP standard were measured in the same manner. Serial diluted standards were added to 100 μL ATP Assay Mix solution, which were kept at RT for 3 minutes. Then 100-μL urine samples were added to each mixture and measurements were conducted.
Data are expressed as means±standard error of the mean. The Student t-test and Mann-Whitney U-test were used for between-group comparisons for parametric and nonparametric data, respectively. The chi-squared test was used for categorical data, and a ROC curve was used to analyze the diagnostic performance of biomarkers for the diagnosis of OAB. Urinary levels of markers according to subgroup and pathogenesis of OAB were analyzed using the Kruskal-Wallis test, while Spearman correlation analyses were used to analyze the relationship between voiding diary parameters, questionnaires, and urinary NGF, PGE2, and ATP. Statistical significance was set at P<0.05, and all statistical tests were 2-sided. IBM SPSS Statistics ver. 20.0 (IBM Co., Armonk, NY, USA) was used to perform all statistical analyses.
In 30 controls and 189 OAB subjects, mean ages were not different between the 2 groups (52.7±1.1 years vs. 54.4±1.0 years, respectively, P=0.277). There was no significant difference in sex ratio between controls and OAB subjects (P=0.526); the percentage of females was 90.0% (27 of 30) and 85.7% (162 of 189) in controls and OAB subjects, respectively. The mean number of micturitions/24 hours was 6.7±0.2 and 12.1±0.2 (P<0.001), and the mean number of urgency episodes/24 hours was 0.1±0.0 and 8.4±0.3 (P<0.001) in controls and OAB subjects, respectively. Mean urinary Cr (mg/dL) was 79.7±8.4 in controls and 75.8±4.3 (P=0.286) in OAB subjects. Finally, the mean OAB-q SF symptom bother score was 20.4±0.4, the mean OAB-q SF HRQL score was 43.1±0.8, and mean OABSS was 8.7±0.2 in OAB subjects.
Mean urinary levels of NGF/Cr were significantly higher in subjects with OAB (1.1±0.1 pg/mg) than in controls (0.2±0.0 pg/mg) (Table 1). Urinary levels of ATP/Cr were also higher, while PGE2/Cr levels tended to be lower in OAB subjects than in controls, though neither comparison showed any statistically significant difference. In the ROC curve (Fig. 1), urinary NGF/Cr was a sensitive biomarker for distinguishing OAB patients (area under the curve [AUC]=0.741; 95% confidence interval [CI], 0.62–0.79; P=0.001). The optimal cut off value was 0.30 pg/mg for urinary NGF/Cr level at Youden index [22]. Using this cut off, the test provided a sensitivity of 63.7% and a specificity of 76.7%. Positive predictive value and negative predictive values were 70.6% and 74.1%, respectively. In the ROC curves of urinary PGE2/Cr and urinary ATP/Cr, no significant results were found (AUC=0.398; 95% CI, 0.299–0.497; P=0.074; AUC=0.608; 95% CI, 0.505–0.711; P=0.058, respectively).
When comparing urinary levels of NGF/Cr, PGE2/Cr, and ATP/Cr with controls according to subgroups and pathogenesis of OAB, urinary levels of NGF/Cr were significantly higher in both OAB-dry (n=117) and OAB-wet (n=72) subgroups than in controls (0.9±0.1, 1.2±0.2, and 0.2±0.0 pg/mg, respectively) (Table 1). Urinary levels of NGF/Cr were also significantly higher in both idiopathic (n=166) and neurogenic (n=23) categories than in controls (1.0±0.1, 1.1±0.3, and 0.2±0.0 pg/mg, respectively) (Table 1). However, urinary levels of PGE2/Cr and ATP/Cr according to subgroup or pathogenesis of OAB did not show a significant difference compared to controls. Spearman correlation analyses demonstrated that only the number of urgency episodes/24 hours was positively correlated with NGF/Cr level (correlation coefficient, 0.156; P<0.05) among relationships between voiding diary parameters, questionnaires, and urinary levels of NGF/Cr, PGE2/Cr, and ATP/Cr (Table 2).
This study demonstrated that urinary levels of NGF/Cr were significantly elevated in OAB patients regardless of subgroup or pathogenesis, and pinpointed its diagnostic performance as a biomarker of OAB. Further, urinary levels of NGF/Cr were correlated with urinary urgency. These results are consistent with previous studies that have proposed urinary NGF as a biomarker of OAB [10-12].
Liu et al. [23] reported that urinary levels of NGF increased with severity of disease in OAB patients, which are categorized as OAB-dry or OAB-wet. Similar to this result, in the current study, the urinary levels of NGF/Cr were significantly elevated in both OAB-dry and OAB-wet patients. Also, the urinary levels of NGF/Cr were significantly raised in both idiopathic and neurogenic OAB. It is suggested that urinary levels of NGF/Cr are significantly higher in OAB patients than in controls regardless of disease subtype or pathogenesis.
Spearman correlation analysis demonstrated that urinary urgency was related to urinary NGF/Cr levels. This finding is consistent with a study by Kim et al. [24] which reported that urinary urgency was the symptom most related to urinary NGF level, but that urinary frequency did not show significant correlation. These results strengthen the position of urinary NGF as a biomarker of OAB, given that urinary urgency is a key symptom of OAB and measuring urinary urgency is essential for diagnosis [25]. The significant positive association was noted only between urinary NGF/Cr and urgency episodes/24 hours, not between urinary NGF/Cr and micturitions/24 hours. The OABSS is sum of frequency, urgency, urge incontinence, and nocturia score [20]. Thus, discrepancy of symptom scores other than urgency score may make the relationship between urinary NGF/Cr and OABSS statistically insignificant. The OAB-q SF also contains several symptoms other than urgency score [21], thus it may result in statistically insignificant results in the relationship between urinary NGF/Cr and OAB-q SF.
Urinary PGE2 levels were significantly higher in OAB patients than in controls compared to previous studies [13,26,27]. Several studies have demonstrated that intravesical instillation of PGE2 led to a decreased bladder capacity and bladder hyperactivity by stimulating the release of tachykinins [28-30]. However, these are not universal findings. In fact, some studies found no significant difference in urinary levels of PGE2 compared with normal controls [24,31], or even lower levels in OAB patients [13]. In the present study, urinary levels of PGE2 were lower in OAB patients compared with controls, though this was not statistically significantly different. Because of the inconsistency of the results, further investigations regarding urinary PGE2 levels are needed.
Urinary ATP has also been proposed as a biomarker for diagnosis of OAB patients [7,16]. Silva-Ramos et al. [7] reported that urinary ATP/Cr was a biomarker for detrusor overactivity in OAB patients. In the current study, urinary ATP/Cr trended higher in OAB subjects than in controls, but did not display a significant difference. This result may come from a relatively wide variation of urinary ATP levels. ATP has a tendency of hydrolyzation in solution if samples are not kept on ice [32]. Thus, samples were preserved at -80˚C to achieve accurate results. Although efforts for achieving accurate results were made, the variation of urinary ATP/Cr level was relatively wide compared with previous studies which reported inconsistent results [7,33]. Wide variation of urinary ATP/Cr may due to a discrepancy in the number of subjects among studies. A larger number of OAB subjects (n=189) were analyzed in the current study than in previous studies; data of 30 female OAB patients and 34 female OAB patients were analyzed in the studies of Sugaya et al. [33] and Silva-Ramos et al [7], respectively. Urinary ATP was positively correlated with bladder distension [34], and it was higher in healthy women compared with age-matched men [7,33]. Limitations of this study include unstandardized degree of bladder distension at the time of urine sampling, as well as the heterogenous sex of subjects. These may be other reasons for wide variation of urinary ATP/Cr. There have been a few studies with inconsistent results regarding urinary ATP/Cr as a biomarker of OAB [32]; thus, further evaluation is required.
Of note, the Promega discontinued NGF Emax ImmunoAssay Systems on March 15, 2014 (during the study period), but evaluation of urinary NGF was not interrupted until the study was completed as our supplies were sufficient. Thus, measurement of NGF was performed consistently with the same kit.
There have been several studies of urinary biomarkers for diagnosis of OAB, many with inconsistent results. The present study demonstrated the potential of urinary NGF/Cr as a biomarker for the diagnosis of OAB. To our knowledge, comparisons of urinary levels of NGF/Cr, PGE2/Cr, and ATP/Cr in the same cohort from the same urine sample have not been performed in previous studies. The relatively wide variation of urinary markers is a limitation of this study. Despite this wide variation, urinary NGF has reliability as previously reported by Vijaya et al. [35]. Reliability is an essential biomarker quality, and therefore this finding is considered to support the appropriateness of using urinary NGF levels for the diagnosis of OAB.
In conclusion, urinary NGF/Cr levels were significantly higher in the OAB group than in the control regardless of disease subgroup or pathogenesis. Urinary NGF/Cr demonstrated appropriate diagnostic performance as a biomarker for the diagnosis of OAB, and its levels correlated with urinary urgency. Urinary NGF/Cr is a potential biomarker that could serve as a basis for the adjunct diagnosis of OAB. Future studies are required to further examine the potential of urinary NGF/Cr as a biomarker for monitoring therapeutic progress in OAB patients.
NOTES
Grant/Fund Support
The research was supported by a Samsung Biomedical Research Institute grant, #SBRI C-B0-227, and a grant of the Korea Health Technology R&D Project through the Korea Health Industry Development Institute (KHIDI), funded by the Ministry of Health & Welfare, Republic of Korea (grant number: HI14C3229).
REFERENCES
1. Stewart WF, Van Rooyen JB, Cundiff GW, Abrams P, Herzog AR, Corey R, et al. Prevalence and burden of overactive bladder in the United States. World J Urol 2003;20:327-36. PMID: 12811491


2. Lee YS, Lee KS, Jung JH, Han DH, Oh SJ, Seo JT, et al. Prevalence of overactive bladder, urinary incontinence, and lower urinary tract symptoms: results of Korean EPIC study. World J Urol 2011;29:185-90. PMID: 19898824


3. Sever N, Oskay U. An investigation of lower urinary tract symptoms in women aged 40 and over. Low Urin Tract Symptoms 2017;9:21-26. PMID: 28120450


5. Liberman JN, Hunt TL, Stewart WF, Wein A, Zhou Z, Herzog AR, et al. Health-related quality of life among adults with symptoms of overactive bladder: results from a U.S. community-based survey. Urology 2001;57:1044-50. PMID: 11377301


6. Lee H, Jeong SJ. Epidemiology of lower urinary tract symptoms: emphasis on the status in Korea. Korean J Urol 2014;55:300-8. PMID: 24868333



7. Silva-Ramos M, Silva I, Oliveira O, Ferreira S, Reis MJ, Oliveira JC, et al. Urinary ATP may be a dynamic biomarker of detrusor overactivity in women with overactive bladder syndrome. PLoS One 2013;8:e64696. PMID: 23741373



8. Steers WD, Tuttle JB. Mechanisms of disease: the role of nerve growth factor in the pathophysiology of bladder disorders. Nat Clin Pract Urol 2006;3:101-10. PMID: 16470209


9. Chuang YC, Fraser MO, Yu Y, Chancellor MB, de Groat WC, Yoshimura N. The role of bladder afferent pathways in bladder hyperactivity induced by the intravesical administration of nerve growth factor. J Urol 2001;165:975-9. PMID: 11176525


10. Antunes-Lopes T, Pinto R, Barros SC, Botelho F, Silva CM, Cruz CD, et al. Urinary neurotrophic factors in healthy individuals and patients with overactive bladder. J Urol 2013;189:359-65. PMID: 23174241


11. Kuo HC, Liu HT, Chancellor MB. Can urinary nerve growth factor be a biomarker for overactive bladder? Rev Urol 2010;12:e69-77. PMID: 20811555


12. Liu HT, Chancellor MB, Kuo HC. Urinary nerve growth factor levels are elevated in patients with detrusor overactivity and decreased in responders to detrusor botulinum toxin-A injection. Eur Urol 2009;56:700-6. PMID: 18472208


13. Kim JC, Park EY, Hong SH, Seo SI, Park YH, Hwang TK. Changes of urinary nerve growth factor and prostaglandins in male patients with overactive bladder symptom. Int J Urol 2005;12:875-80. PMID: 16323980


14. Yamauchi H, Akino H, Ito H, Aoki Y, Nomura T, Yokoyama O. Urinary prostaglandin E₂ was increased in patients with suprapontine brain diseases, and associated with overactive bladder syndrome. Urolog 2010;76:1267 e13-9. 
15. Kumar V, Chapple CC, Chess-Williams R. Characteristics of adenosine triphosphate [corrected] release from porcine and human normal bladder. J Urol 2004;172:744-7. PMID: 15247774


16. Cheng Y, Mansfield KJ, Allen W, Millard RJ, Burcher E, Moore KH. Correlation between cystometric volumes, ATP release, and pH in women with overactive bladder versus controls. Neurourol Urodyn 2013;32:969-73. PMID: 23129360


17. Antunes-Lopes T, Cruz CD, Cruz F, Sievert KD. Biomarkers in lower urinary tract symptoms/overactive bladder: a critical overview. Curr Opin Urol 2014;24:352-7. PMID: 24841379


18. Van Kerrebroeck P, Haab F, Angulo JC, Vik V, Katona F, Garcia-Hernandez A, et al. Efficacy and safety of solifenacin plus tamsulosin OCAS in men with voiding and storage lower urinary tract symptoms: results from a phase 2, dose-finding study (SATURN). Eur Urol 2013;64:398-407. PMID: 23537687


19. Coyne KS, Margolis MK, Hsieh R, Vats V, Chapple CR. Validation of the urinary sensation scale (USS). Neurourol Urodyn 2011;30:360-5. PMID: 21254195


20. Homma Y, Yoshida M, Seki N, Yokoyama O, Kakizaki H, Gotoh M, et al. Symptom assessment tool for overactive bladder syndrome: overactive bladder symptom score. Urology 2006;68:318-23. PMID: 16904444


21. Coyne KS, Thompson CL, Lai JS, Sexton CC. An overactive bladder symptom and health-related quality of life short-form: validation of the OAB-q SF. Neurourol Urodyn 2015;34:255-63. PMID: 25783168


22. Fluss R, Faraggi D, Reiser B. Estimation of the Youden Index and its associated cutoff point. Biom J 2005;47:458-72. PMID: 16161804


23. Liu HT, Tyagi P, Chancellor MB, Kuo HC. Urinary nerve growth factor level is increased in patients with interstitial cystitis/bladder pain syndrome and decreased in responders to treatment. BJU Int 2009;104:1476-81. PMID: 19522864


24. Kim SW, Im YJ, Choi HC, Kang HJ, Kim JY, Kim JH. Urinary nerve growth factor correlates with the severity of urgency and pain. Int Urogynecol J 2014;25:1561-7. PMID: 24866276


25. Park KK, Huh JS. Association of urinary urgency and delay time of micturition in women with overactive bladder. Int Neurourol J 2014;18:150-4. PMID: 25279243



26. Kim JC, Park EY, Seo SI, Park YH, Hwang TK. Nerve growth factor and prostaglandins in the urine of female patients with overactive bladder. J Urol 2006;175:1773-6. PMID: 16600756


27. Cho KJ, Kim HS, Koh JS, Kim JC. Changes in urinary nerve growth factor and prostaglandin E2 in women with overactive bladder after anticholinergics. Int Urogynecol J 2013;24:325-30. PMID: 22717785


28. Ishizuka O, Mattiasson A, Andersson KE. Prostaglandin E2-induced bladder hyperactivity in normal, conscious rats: involvement of tachykinins? J Urol 1995;153:2034-8. PMID: 7752389


29. McCafferty GP, Misajet BA, Laping NJ, Edwards RM, Thorneloe KS. Enhanced bladder capacity and reduced prostaglandin E2-mediated bladder hyperactivity in EP3 receptor knockout mice. Am J Physiol Renal Physiol 2008;295:F507-14. PMID: 18508878


30. Schüssler B. Comparison of the mode of action of prostaglandin E2 (PGE2) and sulprostone, a PGE2-derivative, on the lower urinary tract in healthy women. A urodynamic study. Urol Res 1990;18:349-52. PMID: 2256236


31. Liu HT, Tyagi P, Chancellor MB, Kuo HC. Urinary nerve growth factor but not prostaglandin E2 increases in patients with interstitial cystitis/bladder pain syndrome and detrusor overactivity. BJU Int 2010;106:1681-5. PMID: 19751258


32. Fry CH, Sahai A, Vahabi B, Kanai AJ, Birder LA. What is the role for biomarkers for lower urinary tract disorders? ICI-RS 2013. Neurourol Urodyn 2014;33:602-5. PMID: 24436105



33. Sugaya K, Nishijima S, Kadekawa K, Miyazato M, Mukouyama H. Relationship between lower urinary tract symptoms and urinary ATP in patients with benign prostatic hyperplasia or overactive bladder. Biomed Res 2009;30:287-94. PMID: 19887725


34. Cheng Y, Mansfield KJ, Allen W, Chess-Williams R, Burcher E, Moore KH. ATP during early bladder stretch is important for urgency in detrusor overactivity patients. Biomed Res Int 2014;2014:204604. PMID: 24971316




35. Vijaya G, Cartwright R, Bhide A, Derpapas A, Fernando R, Khullar V. Reliability and validity of urinary nerve growth factor measurement in women with lower urinary tract symptoms. Neurourol Urodyn 2016;35:944-8. PMID: 26227147


Fig. 1.
Receiver-operator characteristics curve for evaluation of the diagnostic performance of urinary NGF/Cr. NGF, nerve growth factor; Cr, creatinine; AUC, area under the curve; CI, confidence interval.
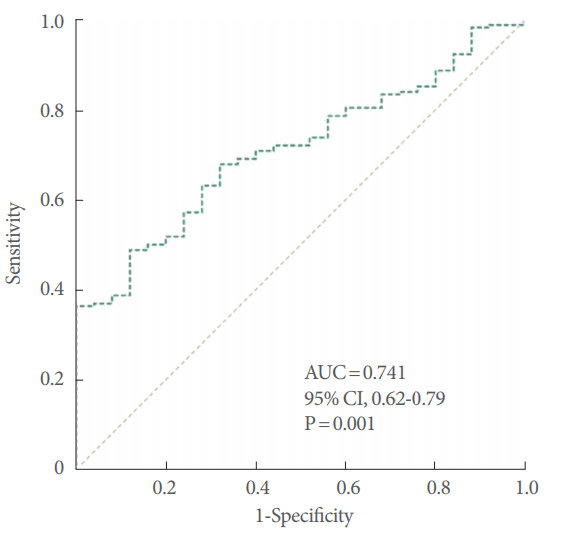
Table 1.
Urinary NGF/Cr, PGE2/Cr, and ATP/Cr levels in controls, OAB subjects, and according to subgroup and pathogenesis of OAB
| Variable | Urinary NGF/Cr (pg/mg) | Urinary PGE2/Cr (pg/mg) | Urinary ATP/Cr (pmol/mg) |
|---|---|---|---|
| Controls (n = 30) | 0.2 ± 0.0 | 19.1 ± 2.3 | 3.7 ± 0.9 |
| OAB subjects (n = 189) | 1.1 ± 0.1* | 16.0 ± 1.0 | 23.1 ± 6.7 |
| Subgroup | |||
| OAB-dry (n = 117) | 0.9 ± 0.1* | 16.7 ± 1.5 | 20.6 ± 4.9 |
| OAB-wet (n = 72) | 1.2 ± 0.2* | 14.9 ± 1.3 | 27.1 ± 15.5 |
| Pathogenesis | |||
| Idiopathic OAB (n = 166) | 1.0 ± 0.1* | 16.0 ± 1.1 | 25.3 ± 7.6 |
| Neurogenic OAB (n = 23) | 1.1 ± 0.3* | 15.6 ± 2.2 | 7.4 ± 3.2 |
Table 2.
Correlation coefficients between voiding diary parameters, questionnaires, and urinary NGF/Cr, PGE2/Cr, and ATP/Cr levels in OAB subjects
| Variable | Micturitions/24 hr | Urgency episodes/24 hr |
OAB-q SF |
OABSS | |
|---|---|---|---|---|---|
| Symptom bother | HRQoL | ||||
| Urinary NGF/Cr (pg/mg) | 0.120 | 0.156* | 0.089 | –0.055 | –0.031 |
| Urinary PGE2/Cr (pg/mg) | –0.058 | 0.001 | –0.030 | –0.098 | 0.056 |
| Urinary ATP/Cr (pmol/mg) | 0.129 | 0.120 | 0.065 | –0.030 | 0.002 |





