Pregnancy With a Successful Vaginal Delivery Following Augmentation Enterocystoplasty for Ketamine Cystitis: A Case Report
Article information
Abstract
A 28-year-old female with a 1-year history of ketamine abuse developed ketamine-associated urinary symptoms that were refractory to conservative treatment after the complete cessation of ketamine use. Smooth voiding with increased bladder capacity and minimal postvoid residual urine volume were achieved by performing an augmentation enterocystoplasty. An uneventful pregnancy with the vaginal delivery of a healthy baby occurred postoperatively.
INTRODUCTION
Ketamine, a dissociative anesthetic agent, is an N-methyl-D-aspartate receptor antagonist. Ketamine abusers presenting with severe dysuria, frequency, urgency, gross hematuria, and suprapubic pain have been reported worldwide since the first description by Shahani et al. [1]. Chung et al. [2] performed augmentation enterocystoplasty (AE) in patients with a contracted bladder capacity of less than 100 mL to relieve refractory ketamine-associated bladder pain and lower urinary tract symptoms. AE has been found to be effective for improving symptoms in patients who have exhibited a sustained cessation of ketamine use. Limited studies of pregnancy with a vaginal delivery or cesarean section after AE have been published [3-5]. Herein, we report the first case of a successful vaginal delivery after AE for ketamine cystitis (KC).
CASE REPORT
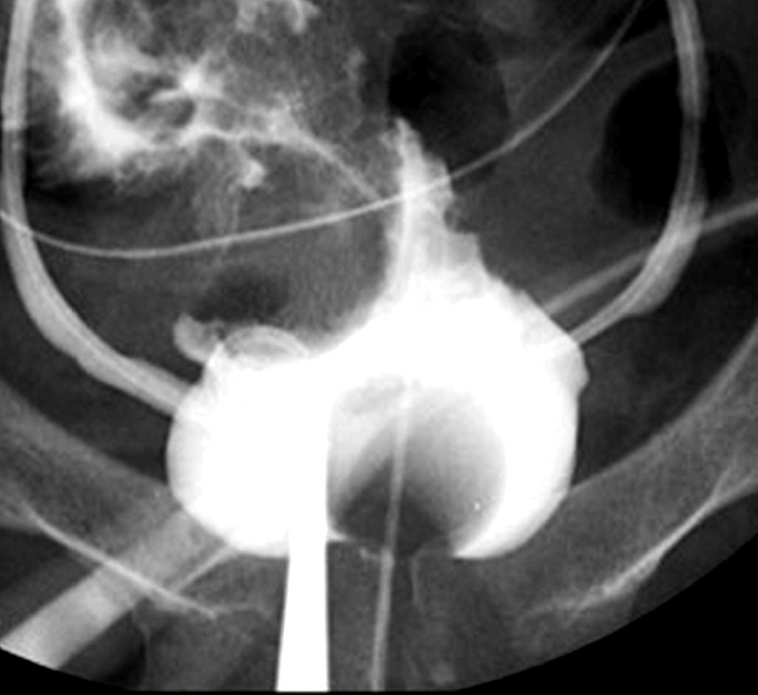
A 28-year-old female abused approximately 5 mg of ketamine daily for 1 year starting at the age of 25. Urinary frequency and bladder pain persisted for a year despite ceasing to use ketamine. She received intravesical hyaluronic acid treatment 11 times 2 years later. She presented to our urology clinic with complaints of urinary frequency, intermittent gross hematuria, lower abdominal pain (pain score, 8 out of 10) and frequent admissions due to acute pyelonephritis. A 2-day voiding diary revealed 27 voiding episodes in 24 hours and a maximum voided volume of 40 mL. No hydronephrosis was detected on renal sonography. A video urodynamic study revealed a contracted urinary bladder (cystometric capacity, 39 mL) without any vesicoureteral reflux. Her baseline serum creatinine level was 0.6 mg/dL (reference range <1.2 mg/dL). A urine culture performed at her first visit showed growth of multidrug-resistant Klebsiella pneumonia, which was managed with oral cephalosporins empirically and according to a drug sensitivity test. Her International Prostate Symptom Score was 35 out of 35. Her bladder capacity increased to 150 mL 1 week postoperatively (Fig. 1). At a 6-month follow-up examination, uroflowmetry showed a bell-shaped curve with a maximum flow rate of 10.3 mL/sec and a voided volume of 144.7 mL. The postvoid residual volume determined using transabdominal sonography was 4.2 mL. Subsequently, she was employed, married, and became pregnant. Her antepartum course was uneventful without symptomatic urinary tract infections (UTIs) or other complications. Regular urinalysis and ultrasonography every 3 months were performed. The patient had an asymptomatic UTI without fever. All urinalysis results showed pyuria, bacteriuria, and positive results for leukocyte esterase. She vaginally delivered a healthy male infant, 3,600 g in weight, 1.5 years after AE. No febrile UTI or urinary incontinence was noted at a 3-year follow-up.
DISCUSSION
This case demonstrates that sustained abstinence from ketamine allowed a successful AE procedure and led to a promising life with a pregnancy and successful vaginal delivery. Effective AE for irreversible KC contributes to increased bladder capacity, minimal postvoid residual urine volume, decreased incidence of febrile UTIs, and significant relief of bladder pain [2]. Resuming normal social life is feasible with an improved quality of life.
The current consensus on the effective treatment of KC is absolute abstinence from ketamine use. Continuing users must set complete cessation of ketamine use as the ultimate goal for AE to be successful, since symptoms can flare up after the reuse of ketamine postoperatively [2]. Before proceeding to a surgical intervention for irreversible KC, serum creatinine levels, renal sonography, uroflowmetry, and postvoid residual urine volume by ultrasound should be evaluated. A cutoff value for the maximal bladder capacity of less than 100 mL has been suggested for AE [2]. According to Chung et al. [2] , all 14 patients who underwent AE for KC had a bladder volume less than 100 mL. The bladder volume of the other 4 patients undergoing AE for KC reported by Ng et al. [6] was less than 50 mL. Therefore, the review article published by Jhang et al. [7] suggested that patients with KC should undergo AE if their bladder capacity is less than 100 mL with low bladder compliance. In our experience, AE for neurogenic bladder due to tethered cord syndrome usually increases the bladder volume to 400 mL. This outcome has not been obtained in AE for KC. In the series published by Chung et al. [2], the mean cystometric bladder capacity increased to 309.2±58.0 mL 3 to 6 months postoperatively. However, the poorest outcome was only 200 mL. In the series published by Ng et al. [6], 2 patients had a bladder volume greater than 400 mL. However, the other 2 cases exhibited much smaller bladder volumes. One was 250 mL 30 months after AE, and the other one was 150 mL 6 months after AE. We did not remove the original bladder during AE. The remaining hypersensitive bladder in patients with KC might make the patients feel the urge to urinate more frequently than those with neurogenic bladder, who usually do not have intact bladder sensation.
Only a few case reports dealing with pregnancy and delivery after AE have been published [3-5]. Pregnancy after AE is no longer a novel topic, but this is the first reported case of an exketamine abuser with a successful pregnancy after AE. The first pregnancy following AE for tubercular cystitis was described in 1955. Most of the reported cases had the underlying disease of neurogenic bladder related to spinal problems [4]. Approximately 50%–100% of patients with AE had asymptomatic bacteriuria, but only 4%–43% exhibited significant UTIs [8]. However, the risk of UTIs in pregnancy is greater due to anatomical changes. Regular antepartum urinalysis is indicated to ensure that all symptomatic infections are treated promptly. This prevents premature labor resulting from pyelonephritis. Serial renal function tests and renal sonography to detect hydronephrosis should also be performed. Assessing each patient individually guides the management of labor. Even given the anatomical alterations that take place after AE, vaginal delivery is feasible for those with a normal continence mechanism [3,4]. A cesarean section is indicated for patients who undergo AE with bladder neck reconstruction. A urologist familiar with the anatomy of AE should be present to assist with cesarean sections in such patients.
This case report demonstrated that a promising life with pregnancy and a vaginal delivery is possible following ketamine cessation and successful AE for ketamine-related bladder contracture.
Notes
Conflict of Interest
No potential conflict of interest relevant to this article was reported.