|
 |


- Search
| Int Neurourol J > Volume 20(2); 2016 > Article |
|
ABSTRACT
Purpose:
The purpose of this study was to determine the prevalence of urinary incontinence (UI) and analyze its association with instrumental activities of daily living (IADL) and benign prostatic hyperplasia (BPH) in community-dwelling older men in Korea.
Methods:
This study was a secondary analysis of data from the Actual Living Condition of the Elderly and Welfare Need Survey conducted in the year 2008. Data was subjected to hierarchical logistic regression analysis to examine the association of IADL and BPH with UI in older men, entering IADL and BPH in model 1, and age, body mass index (BMI) and education in model 2, and then comorbidities and walking speed in model 3.
Results:
Of 6,185 men, 243 (3.9%) had self-reported UI. The prevalence of UI was 1.8% in men aged 60–64 years and 11.7% in those aged 85 years and above, indicating an increase in the prevalence of UI with their age. IADL and BPH remained the only significant factors associated with UI in model 1 (odds ratio [OR], 1.54; 95% confidence interval [CI], 1.44–1.64 and OR, 2.73; 95% CI, 1.47–5.10, respectively), model 2 (OR, 1.50; 95% CI, 1.40–1.61 and OR, 2.68; 95% CI, 1.42–5.07), and model 3 (OR, 1.43; 95% CI, 1.32–1.54 and OR, 2.58; 95% CI, 1.36–4.90).
Conclusions:
IADL limitations and presence of BPH were associated with UI in older men after controlling for BMI, education, comorbidities, and walking speed. Thus, UI should be assessed in older Korean men with IADL decline and BPH. Gender-sensitive interventions to attenuate IADL limitations and manage BPH should be developed and applied to improve UI in older men.
Urinary incontinence (UI), defined as “the complaint of involuntary loss of urine”, [1] is a common condition negatively affecting the quality of life in older adults [2]. The overall prevalence of UI in older men ranges from 13% to 17% in literature from Western countries [3,4]. In Japan, the prevalence of UI was found to be 13.7% in men aged 30 years and above, 15% in men aged 60–70 years, and 22% in men older than 70 years [5]. Despite variations in the reported prevalence of UI in older men as seen in studies from different parts of the world, a consistent increase in prevalence of UI with older adults’ age is observed [3,5,6].
Urgency UI is the most prevalent type of UI in men [7,8]. The prevalence of urgency UI in men aged 60 years and above was found to be 2.5%, while the prevalence of mixed and stress UI in the same age group were 1.2% and 1.6%, respectively [8]. Among Japanese men, 6.3% had urgency UI, which is 2.5 times higher than their prevalence of stress UI [5]. Similarly, in Korea, a population-based study reported the prevalence of UI to be 11.6% in men aged 60 years and above, with 6.2% of men reporting urgency UI, making it the most prevalent type of UI [9].
Risk factors for UI in older men include advanced age, diabetes mellitus (DM), hypertension, problems with memory, stroke, functional impairment and benign prostatic hyperplasia (BPH) [6,7,10-13]. Among these factors, functional impairment and BPH have higher odds of being associated with UI [6]. There is limited information on the prevalence of UI and factors associated with it among older men in the Korean context. The purpose of this study, therefore, was to determine the prevalence of UI and to analyze its association with instrumental activities of daily living (IADL) and BPH in communitydwelling older men in Korea.
Data pertaining to a total of 6,185 men aged 60 years and above, who participated in the 2008 Actual Living Condition of the Elderly and Welfare Need Survey conducted by the Korean Ministry of Health and Welfare, was analyzed for this study. A total of 15,146 individuals aged 60 years or older (male, 6,185; female, 8,961) were interviewed for the 2008 dataset, but we only selected the male participants for this study. This survey began in 2008, and data was collected to explore population-based information about the living conditions and welfare needs of older Koreans. Deidentified raw dataset of the survey was obtained from the Korean Institute for Health and Social Affairs after registering the study with them. This study was approved by the Institutional Review Board of Hanyang University (approval number: HY-15-085-1).
The following demographic data were analyzed: age, body mass index (BMI) and educational level expressed as number of years of education (0–3, 4–6, ≥7). Hypertension, DM, stroke, BPH and depression, which were medically diagnosed, were included in the analysis.
Study participants answering “Yes” to the question “Do you have UI?” were defined as having UI.
To measure the number of IADL, participants were asked about their ability to care for their body, use the telephone, go shopping, prepare food, do housekeeping, go out of the house without transportation, do laundry, manage transportation, take responsibility for their own medications, and handle finances. The responses to choose IADL items including the ability to use the telephone, go shopping, and manage transportation were “totally independent,” “need little help,” “need a lot of help,” or “totally dependent.” Responses to the other questions could be “totally independent,” “need help”, and “totally dependent.” A response of “totally independent” was considered to indicate that the individual was not limited for that particular IADL. The total number of limited IADL had a possible range of 0–10 with a higher score indicating a higher level of dependence. This score was analyzed for association with UI.
Descriptive statistics including mean, standard deviation (SD), frequency and percentages were used to summarize the general characteristics of the participants. To examine the association between IADL and BPH, and UI, a hierarchical logistic regression model was developed. Model 1 included IADL and BPH. In model 2, demographic variables including age, BMI, and education were added to model 1. In model 3, comorbidities including hypertension, DM, stroke and depression, and walking speed were added to model 2. Statistical analyses were performed using IBM SPSS Statistics version 20.0 (IBM Co., Armonk, NY, USA) and a P-value of less than 0.05 was considered statistically significant.
The general characteristics of all study subjects are presented in Table 1. Mean age of participants was 70.4 years (SD, ±6.7). Approximately half of all study participants had 7 years or more of education while 35% had 4–6 years of education. Fifty-two percent of participants were either overweight or obese while only 5.5% were underweight based on BMI values. Hypertension (39%) and depression (24%) were the most common comorbidities. Only 7.2% of participants had BPH, making it the least common health problem in the study population. The mean limited IADL score was 0.9 (SD, ±2.3), while the mean walking speed for 2.5 m was 3.9 seconds (SD, ±1.5).
Results of hierarchical logistic regression analysis to determine the association between IADL and BPH with UI are presented in Table 3. In model 1, both IADL and BPH were significantly associated with the presence of UI (OR, 1.54; 95% CI, 1.44–1.64 and OR, 2.73; 95% CI, 1.47–5.10, respectively). There was a proportional increase in the OR for UI with the number of limited IADL. Men with BPH were more likely to have UI than men without BPH. Model 2 incorporated age, BMI, and education in addition to IADL and BPH. Both IADL (OR, 1.50; 95% CI, 1.40–1.61) and BPH (OR, 2.68; 95% CI, 1.42–5.07) remained significant factors for UI. The odds ratios for these factors were slightly lower than in model 1. In model 3, comorbidities including hypertension, DM, stroke and depression, and walking speed were added to model 2. Both IADL (OR, 1.43; 95% CI, 1.32–1.54) and BPH (OR, 2.58; 95% CI, 1.36–4.90) were still significantly associated with UI, although the odds ratios were slightly lower than in models 1 and 2. No other factors were found to be significantly associated with UI.
We determined the prevalence of UI in community-dwelling elderly men in Korea and analyzed associated factors, with a particular focus on IADL and BPH. The overall prevalence of UI in older men was 3.9%, which is lower than that reported in previous studies [8,9]. The EPIC study [8] analyzing data from five countries including Canada, Germany, Italy, Sweden and the UK reported an overall prevalence of 10.4% for UI in older men. Similarly, Kim et al. [9] reported a prevalence of 11.6% for UI in Korean men. A possible explanation for the wide disparity between the current study and the previous studies could be related to the use of different definitions for UI. In the current study, participants were considered as having UI if they answered “Yes” to the question “Do you have UI?”. The two studies cited [8,9] used the 2002 International Continence Society definition of UI as participants having “complaints of any involuntary leakage of urine.” With approximately 51% of participants in the current study having less than 7 years of education, it is possible that they may have failed to understand the question asked regarding UI. This factor could have contributed to the low prevalence of UI in our study. Future studies should carefully select a valid and reliable question to assess UI among older adults.
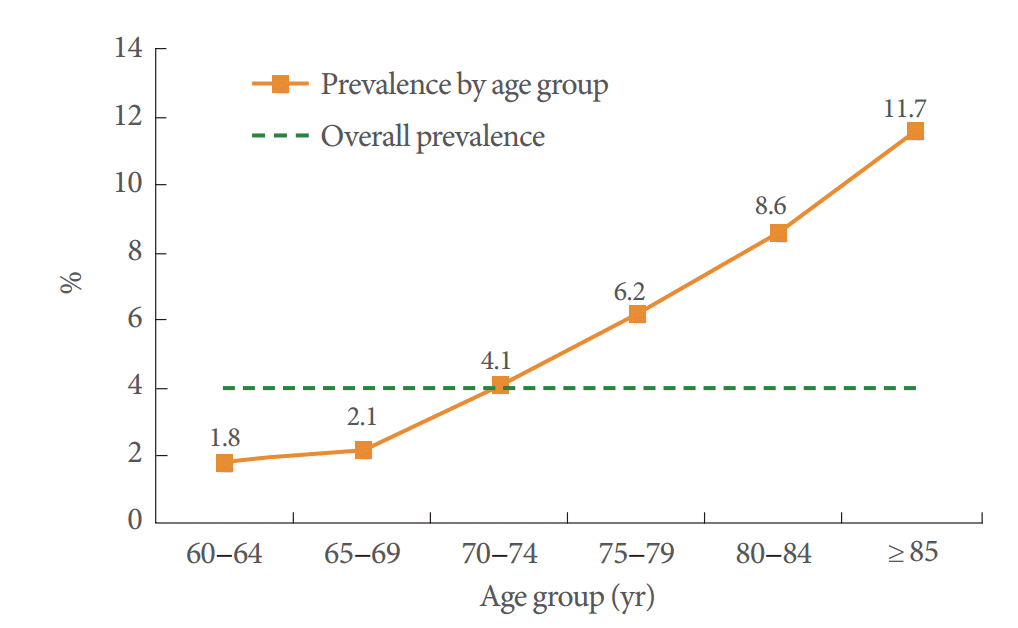
It is well established that the prevalence of UI increases with advanced age. Previous studies found that the prevalence of UI was higher in men aged 40 years and above [5,8,9]. However, there is limited information about its prevalence in different age groups in older Korean men. Anger et al. [3] found an increasing prevalence of UI starting from the age of 60 years. They reported a prevalence rate of 11% for UI in men aged 60–64 years and 31% in men aged 85 years and above. Prevalence of lower urinary tract symptoms (LUTS) in men was 10.6% in the age group 45–49 years compared to 35.4% in those over 80 years [14]. Such a difference between age groups has not been reported in older women [15]. Our findings were consistent with these studies with respect to UI with prevalence rates of 1.8% in the age group 60 and 11.7% for those aged 85 years and above. To summarize, prevalence of UI increases consistently with advanced age regardless of race or country of origin.
We also found that limitations in IADL and presence of BPH were significantly associated with UI in older men. This remained true even after controlling for demographic factors, comorbidities, and walking speed. These findings were consistent with results from previous studies. A 2-year longitudinal population based study found UI to be a significant predictor of IADL decline in both men and women [11]. In addition, a systematic review involving pooled analysis of four studies reported that older men with impaired activities of daily living (ADL) scores had increased odds of having UI [6]. Here, we would like to point out an important research question: should ADL scores and IADL scores be used as predictors or outcomes of UI? Majority of studies consider UI to be a predictor of functional ability, such as ADL and IADL, among older adults. Because our study was based on a cross-sectional design, we could not evaluate whether a higher level of dependency for IADL had an impact on UI in older men. It should be noted, however, that IADL scores are emerging as strong predictors of UI in older men. This has potential implications for health care professionals in recognizing the need to develop interventions focusing on improving independence for IADL in community-dwelling older men.
Urgency UI, which is the most prevalent type of UI in older men [5,8,9], is often related to bladder outlet obstruction secondary to BPH. Markland et al. [4] found that BPH was significantly associated with moderate and severe UI in men aged 40 years and above. The increasing prevalence of BPH seen in Korea reflects its rapidly increasing elderly population. The prevalence of clinical diagnosis of BPH in the 2011 Actual Living Condition of the Elderly Survey was 16.5% [16], which is much higher than the prevalence rate of 7.2% recorded in a similar national survey conducted in 2008. This trend suggests that BPH is emerging as a serious health problem in older men and a corresponding increase in the prevalence of UI secondary to BPH is expected in the near future. Against this background, it is important to consider preventive interventions to reduce the risk of symptomatic BPH, LUTS, and UI. Previous studies have reported that obesity [17,18], physical activity [19,20], and diet [21] have a significant effect on the risk of BPH and LUTS. In particular, there is evidence of a positive correlation between BMI and risk of BPH [22]. We found that more than half of the men in our study were either overweight or obese. Therefore, it may be necessary to develop and apply interventions to modify health behavior towards maintaining optimal body weight.
The strength of the current study is the generalizability of the findings as data for this study was sourced from a sample representative of the entire population of Korea. However, we could not establish a causal relationship between UI and its associated factors owing to the cross-sectional design of the study. Another limitation of this study was that severity and types of UI were not included in the analysis because of the lack of such information in the dataset.
This study has multiple implications for health professionals. Only 9% of older Korean men compared to 25.9% of older European men sought medical treatment for UI [15]. A similar trend was seen in older Korean women who had a low rate of seeking medical treatment for UI [23]. This may be attributed to cultural differences between the two regions on how UI is perceived by older adults. UI is considered to be a normal agerelated change, in general, and therefore educational programs to address knowledge and attitude gaps concerning UI are needed for older adults as well as health care professionals in Korea. In addition, there is a need for gender-specific instruments for screening and assessing UI in older men as there are differences between men and women with respect to the prevalence and types of UI. Though the International Prostate Symptom Score (IPSS) has been widely utilized in research as well as in clinical settings for men, its application is mostly limited to assessing patients with LUTS due to BPH. Moreover, IPSS has limitations in determining the type of UI. A simple, reliable and valid tool to assess UI in older men is needed.
In conclusion, the prevalence of UI in our study population increased with age. However, the prevalence of UI in older men is lower in Korea than that reported from other countries. IADL and BPH were identified as factors significantly associated with UI. They remained significant even after controlling for demographic factors, comorbidities, and walking speed. The prevalence of BPH in the current study might be lower than the actual prevalence because of the low educational status and the use of self-reported questionnaire in defining the population having UI.
NOTES
REFERENCES
1. Haylen BT, de Ridder D, Freeman RM, Swift SE, Berghmans B, Lee J, et al. An International Urogynecological Association (IUGA)/International Continence Society (ICS) joint report on the terminology for female pelvic floor dysfunction. Neurourol Urodyn 2010;29:4-20. PMID: 19941278


2. Guzelsoy M, Demirci H, Coban S, Belkiz Gungor B, Ustunyurt E, Isildak S. Impact of urinary incontinence on quality of life among residents living in Turkey. Urol J 2014;11:1447-51. PMID: 24807758

3. Anger JT, Saigal CS, Stothers L, Thom DH, Rodriguez LV, Litwin MS, et al. The prevalence of urinary incontinence among community dwelling men: results from the National Health and Nutrition Examination survey. J Urol 2006;176:2103-8. PMID: 17070268


4. Markland AD, Goode PS, Redden DT, Borrud LG, Burgio KL. Prevalence of urinary incontinence in men: results from the national health and nutrition examination survey. J Urol 2010;184:1022-7. PMID: 20643440


5. Yoshimura K, Nakayama T, Sekine A, Matsuda F, Kosugi S, Sugino Y, et al. Prevalence of postmicturition urinary incontinence in Japanese men: comparison with other types of incontinence. Int J Urol 2013;20:911-6. PMID: 23305565


6. Shamliyan TA, Wyman JF, Ping R, Wilt TJ, Kane RL. Male urinary incontinence: prevalence, risk factors, and preventive interventions. Rev Urol 2009;11:145-65. PMID: 19918340


7. Buckley BS, Lapitan MC; Epidemiology Committee of the Fourth International Consultation on Incontinence, Paris, 2008. Prevalence of urinary incontinence in men, women, and children--current evidence: findings of the Fourth International Consultation on Incontinence. Urology 2010;76:265-70. PMID: 20541241


8. Irwin DE, Milsom I, Hunskaar S, Reilly K, Kopp Z, Herschorn S, et al. Population-based survey of urinary incontinence, overactive bladder, and other lower urinary tract symptoms in five countries: results of the EPIC study. Eur Urol 2006;50:1306-14. PMID: 17049716


9. Kim TH, Han DH, Lee KS. The prevalence of lower urinary tract symptoms in Korean men aged 40 years or older: a population-based survey. Int Neurourol J 2014;18:126-32. PMID: 25279239



10. Goode PS, Burgio KL, Redden DT, Markland A, Richter HE, Sawyer P, et al. Population based study of incidence and predictors of urinary incontinence in black and white older adults. J Urol 2008;179:1449-53. PMID: 18295279



11. Holroyd-Leduc JM, Mehta KM, Covinsky KE. Urinary incontinence and its association with death, nursing home admission, and functional decline. J Am Geriatr Soc 2004;52:712-8. PMID: 15086650


12. Koskimaki J, Hakama M, Huhtala H, Tammela TL. Association of non-urological diseases with lower urinary tract symptoms. Scand J Urol Nephrol 2001;35:377-81. PMID: 11771864


13. Omli R, Hunskaar S, Mykletun A, Romild U, Kuhry E. Urinary incontinence and risk of functional decline in older women: data from the Norwegian HUNT-study. BMC Geriatr 2013;13:47. PMID: 23678851




14. Smith DP, Weber MF, Soga K, Korda RJ, Tikellis G, Patel MI, et al. Relationship between lifestyle and health factors and severe lower urinary tract symptoms (LUTS) in 106,435 middle-aged and older Australian men: population-based study. PLoS One 2014;9:e109278. PMID: 25333345



15. Boyle P, Robertson C, Mazzetta C, Keech M, Hobbs FD, Fourcade R, et al. The prevalence of lower urinary tract symptoms in men and women in four centres. The UrEpik study. BJU Int 2003;92:409-14. PMID: 12930430


16. Korean Statistical Information Service. Self-reported prevalence of chronic diseases by sex in the Korean elderly [Internet]. Daejeon: Korean Statistical Information Service; c2014 [updated 2015 May 7; cited 2015 Aug 18]. Available from: http://kosis.kr/statHtml/statHtml.do?orgId=117&tblId=DT_11771_2011N036.
17. Kristal AR, Arnold KB, Schenk JM, Neuhouser ML, Weiss N, Goodman P, et al. Race/ethnicity, obesity, health related behaviors and the risk of symptomatic benign prostatic hyperplasia: results from the prostate cancer prevention trial. J Urol 2007;177:1395-400. PMID: 17382740


18. Rohrmann S, Smit E, Giovannucci E, Platz EA. Association between markers of the metabolic syndrome and lower urinary tract symptoms in the Third National Health and Nutrition Examination Survey (NHANES III). Int J Obes (Lond) 2005;29:310-6. PMID: 15672112


19. Dal Maso L, Zucchetto A, Tavani A, Montella M, Ramazzotti V, Polesel J, et al. Lifetime occupational and recreational physical activity and risk of benign prostatic hyperplasia. Int J Cancer 2006;118:2632-5. PMID: 16380994


20. Parsons JK, Kashefi C. Physical activity, benign prostatic hyperplasia, and lower urinary tract symptoms. Eur Urol 2008;53:1228-35. PMID: 18358592


21. Bravi F, Bosetti C, Dal Maso L, Talamini R, Montella M, Negri E, et al. Macronutrients, fatty acids, cholesterol, and risk of benign prostatic hyperplasia. Urology 2006;67:1205-11. PMID: 16765180


22. Wang S, Mao Q, Lin Y, Wu J, Wang X, Zheng X, et al. Body mass index and risk of BPH: a meta-analysis. Prostate Cancer Prostatic Dis 2012;15:265-72. PMID: 22183774


23. Park J, Hong GR, Yang W. Factors associated with self-reported and medically diagnosed urinary incontinence among community-dwelling older women In Korea. Int Neurourol J 2015;19:99-106. PMID: 26126439



Table 1.
General characteristics of participants
| Variable | Value |
|---|---|
| Age (yr) (n = 6,185) | 70.4 ± 6.71 |
| Education (yr) (n = 6,064) | |
| 0–3 | 928 (15.3) |
| 4–6 | 2,149 (35.4) |
| ≥7 | 2,987 (49.3) |
| Body mass index (kg/m2)a) (n = 5,679) | |
| Underweight ( < 18.5) | 311 (5.5) |
| Normal (18.5–22.9) | 2,411 (42.45) |
| Overweight (23–24.9) | 1,513 (26.6) |
| Obese ( ≥ 25) | 1,444 (25.4) |
| Comorbidities | |
| Hypertension (n = 6,185) | 2,422 (39.2) |
| Diabetes mellitus (n = 6,185) | 923 (14.9) |
| Stroke (n = 6,185) | 480 (7.8) |
| Benign prostatic hyperplasia (n = 6,185) | 444 (7.2) |
| Depression (n = 6,113) | 1,450 (23.7) |
| No. of limited IADL (n = 6,185) | 0.85 ± 2.25 |
| Walking speed in seconds (n = 4,617) | 3.87 ± 1.51 |
Table 2.
Prevalence of urinary incontinence by age groups in older Korean men
| Age (yr) | Prevalence, n (%) |
|---|---|
| 60–64 | 23 (1.8) |
| 65–69 | 36 (2.1) |
| 70–74 | 65 (4.1) |
| 75–79 | 59 (6.2) |
| 80–84 | 36 (8.6) |
| ≥ 85 | 24 (11.7) |
| Overall | 243 (3.9) |
Table 3.
Association of IADL and BPH with urinary incontinence in older Korean men
| Variable | Model 1 | Model 2 | Model 3 |
|---|---|---|---|
| No. of limited IADL | 1.54 (1.44-1.64)*** | 1.50 (1.40-1.61)*** | 1.43 (1.32-1.54)*** |
| BPH | 2.73 (1.47-5.10)** | 2.68 (1.42-5.07)** | 2.58 (1.36-4.90)* |
| Age (yr) | |||
| 60-64 | - | Reference | Reference |
| 65-69 | - | 1.44 (0.61-3.39) | 1.35 (0.57-3.19) |
| 70-74 | - | 1.26 (0.53-3.01) | 1.13 (0.47-2.71) |
| 75-79 | - | 1.71 (0.69-4.21) | 1.50 (0.60-3.71) |
| 80-84 | - | 2.09 (0.77-5.63) | 1.73 (0.63-4.74) |
| ≥85 | - | 3.19 (1.06-9.54) | 2.99 (0.99-9.01) |
| Body mass indexa) (kg/m2) | |||
| Underweight | - | 1.40 (0.62-3.13) | 1.46 (0.65-3.30) |
| Normal | - | Reference | Reference |
| Overweight | - | 0.57 (0.30-1.12) | 0.57 (0.29-1.11) |
| Obese | - | 1.11 (0.63-1.95) | 1.00 (0.56-1.79) |
| Education (yr) | |||
| 0-3 | - | Reference | Reference |
| 4-6 | - | 1.37 (0.69-2.70) | 1.38 (0.70-2.72) |
| ≥7 | - | 1.19 (0.60-2.37) | 1.24 (0.62-2.46) |
| Comorbidities | |||
| Hypertension | - | - | 1.27 (0.78-2.06) |
| Diabetes mellitus | - | - | 1.36 (0.75-2.49) |
| Stroke | - | - | 1.66 (0.85-3.23) |
| Depression | - | - | 1.36 (0.81-2.27) |
| Walking speed | - | - | 1.14 (0.99-1.31) |
Values are presented as odds ratio (95% confidence interval).
IADL, instrumental activities of daily living; BPH, benign prostatic hyperplasia.